Research | April 2010 Hearing Review
Correlations between dispensing protocols and successful patient outcomes
Although it is apparent that hearing aids have improved significantly during the past decade, the data indicate that quality control at the point of dispensing has not kept pace with technological improvements.

|
| This article was submitted to HR by Sergei Kochkin, PhD, executive director of the Better Hearing Institute, Washington, DC; Douglas L. Beck, AuD, director of professional relations, Oticon Inc, Somerset, NJ; Laurel A. Christensen, PhD, vice president of research and development, GN ReSound Group, Glenview, Ill; Cynthia Compton-Conley, PhD, professor and director, Assistive Devices Center, Gallaudet University, Washington, DC; Brian J. Fligor, ScD, director of diagnostic audiology, Children’s Hospital Boston, and instructor in otology and laryngology, Harvard Medical School; Patricia B. Kricos, PhD, professor of audiology, University of Florida, Gainesville; Jay B. McSpaden, PhD, retired audiologist and hearing instrument specialist, Jefferson, Ore; H. Gustav Mueller, PhD, professor, Vanderbilt University, Nashville, Tenn; Michael J. Nilsson, PhD, vice president of auditory research, Sonic Innovations Inc, Salt Lake City; Jerry L. Northern, PhD, director of professional services, special projects in education and training, Starkey Laboratories, Eden Prairie, Minn; Thomas A. Powers, PhD, vice president of audiology and compliance, Siemens Hearing Instruments, Inc, Piscataway, NJ; Robert W. Sweetow, PhD, director of audiology and professor of otolaryngology, University of California, San Francisco; Brian Taylor, AuD, professional development manager, Unitron, Plymouth, Minn; and Robert G. Turner, PhD, professor in the Department of Communication Disorders, Louisiana State University, New Orleans. |
In previous articles within this series,1,2 it was quantified that in the United States the hearing loss population has grown to 34.25 million people. Approximately 25% of people with hearing loss own hearing aids, and the majority of hearing aid owners have moderate-to-severe hearing loss.
In the last generation, little progress has been made in regard to the proportion of patients who are “satisfied” or “very satisfied” with their hearing aids. Likewise, hearing aids “in the drawer” (hearing aids never used) have varied between 11.7% and 17.9% and are currently 12.4% representing more than 1 million patients. The key reasons for hearing aids in the drawer include: poor benefit, poor fit and comfort, and unsatisfactory performance in noise.3 Additionally, the last generation has witnessed little progress in terms of positive-word-of-mouth endorsement of hearing aids by patients, and despite the “digital revolution,” more than half of all patients who own hearing aids would not repurchase their current brand of hearing aids.1
In a previous paper,4 we quantified that more than 4 million people, who could benefit from hearing aids, will not purchase them because of the poor experience of their friends and relatives. Hearing aid return rates (ie, return for credits, RFC) remain high5 and, according to surveys with patients, appears to be partly due to: poor benefit (51%), hearing aid performance in noise (49%), whistling/feedback (38%), poor value (36%), and poor fit and comfort (35%).4
Although it is apparent that hearing aids have improved and benefitted significantly from the digital revolution, technological improvements, and highly flexible fitting software, it is our thesis that quality control at the point of dispensing has not kept pace with technological improvements. Indeed, there is great variability in the hearing aid fitting process, and it appears that critical aspects of the fitting protocol are not followed6 despite general consensus among all the professional societies (AAA, ASHA, IHS),7-10 consumer-based advocate groups representing patients, such as The Hearing Loss Association of America (HLAA),11 the Hearing Industries Association (HIA),12 the US Food and Drug Administration,13 and Consumer Reports.14
If we were to simplify the “common sense” process to fitting hearing aids, the process would involve:
- Physical evaluation/examination of the ear and a review of the patent’s history;
- Acquisition of reliable and valid measures of the patient’s hearing loss;
- Selection of the correct technology for the patient, including availability of a telecoil in the hearing aid;
- Assessment of expectations and establishment of realistic expectations;
- Performing quality control measures of the hearing aids prior to fitting using a hearing aid analyzer;
- Determining the required valid gain and output prescription and verifying via real-ear measurement (REM) with probe microphones;
- Fine-tuning the hearing aid fitting with available software based on patient input as well as the use of patient-specific behavioral measures, such as Loudness Discomfort Levels (LDLs) and Acceptable Noise Levels (ANLs), etc;
- Validating that the patient’s treatment with hearing aids has been effective by comparing pre- and-post measures of speech or sentence comprehension in noise and quiet and using real-world performance metrics; and
- Providing counseling and aural rehabilitative services relative to the patient’s specific needs, including care and maintenance of the hearing aid and instruction on hearing aid features, such as how to use the telecoil in the hearing aid.
Some of the key mistakes, in rank order of importance, made by clinicians were summarized in a presentation by Christensen and Groth15 at the 2008 convention of the American Academy of Audiology (AAA):
- Failing to verify the fitting with probe-microphone measurements;
- Understanding when to use an open fitting and when not to;
- Assuming the manufacturer defaults are correct for each patient;
- Not taking manual dexterity into account when selecting the hearing aids;
- Not performing appropriate validation measures;
- Not conducting the appropriate counseling;
- Using the first-time, new-user, or inexperienced-user gain settings and not revisiting the settings over time;
- Fitting a hearing aid without “buy-in” from the patient;
- Assuming that automatic environmental steering programs are accurate and the hearing aids switch appropriately; and
- Failing to use newer tests to help with selection, fitting, and counseling.
The primary mistake according to the authors15 was non-use of probe-microphone real-ear measurement (REM) by audiologists and hearing instrument specialists to objectively quantify the acoustic output or gain of the hearing aids in the patient’s ear canal. REM is objective and accurate, and offers a more meaningful metric than measures of functional gain. These measures are critical for assessing audibility, appropriate output for different input levels, and verification of prescriptive algorithms.
Indeed, a most compelling reason for REM is that several studies16-19 have confirmed that the manufacturer’s initial-fit algorithm often is an inadequate amplification prescription, sometimes providing less-than-prescribed gain in the high frequencies by as much as 20 dB. A study conducted in England20 confirmed these findings and found an 18% improvement in patient satisfaction for those fit using REM versus those not fit with REM.
Despite the clear and recognized importance of REM in fitting hearing aids, The Hearing Review 2006 Dispenser Survey6 showed that, although 57% of dispensing offices owned REM equipment, only 23% used REM routinely during adult hearing aid fittings. The Hearing Journal 2006 dispenser survey21 confirmed that 30.7% of audiologists and 34% of hearing instrument specialists use REM “most of the time” or “always/nearly always.”
Why is REM not used routinely? A number of reasons have been proposed22-23: high cost of equipment, space demands, time needed to perform the testing, cumbersome nature of the REM equipment, an uncertain correlation with hearing aid satisfaction, a misguided belief that REM cannot be used with digital hearing aids, over-reliance on the manufacturers’ “first-fit” algorithms, the belief that fitting software graphics are a good substitute for REM, failure of training programs to emphasize the need for real-ear verification, lack of best practices in clinics where graduates are placed, lack of dedication to best practices by some practitioners, the belief that procedures such as fitting the hearing aid in a soundfield or speech mapping without probe microphones are superior to REM.
While the focus of this review primarily focused on probe-mic verification, there are many other components of a complete fitting protocol, which also seem to be neglected, including: testing in a sound booth, aural rehabilitation, use of a hearing aid analyzer to assess the functionality of the hearing aid, and validation of the hearing aid fit.6 In informal polls by the principal author with dispensers as to why they do not routinely verify or validate the hearing aid fit, the most candid answers received were: “We just don’t want to know” and “What should I do if I cannot find any benefit? Return the money to the patient?”
Others expressing more “politically correct” opinions have indicated there is no compelling scientific evidence to perform all of the components of the hearing aid fitting protocol. For example, they point out some researchers24 have shown that there is no measurable advantage to fine-tuning the hearing aid gain and output for new users beyond the initial fit where the adjustment is 10 dB or less. One study25 using two fitting protocols (where REM was used in both protocols) withheld the use of loudness discomfort measurement and speech-in-noise testing. The authors found no significant differences between the two samples.
An Optometric Analogy: Does Protocol Matter?
When patients go to a vision-chain outlet for eyeglasses, there is little variability in the protocol for fitting corrective lenses. The patient is led through five or six stations by a technician, and at the end the patient has a reasonable approximation of their vision correction needs. Arguably, the most important test seems to be the direct reading of the retina’s response to a beam of light shot at it. Following this analysis, the optometrist makes fine adjustments using patient input/observation and validates the accuracy of the prescription by asking the patient to read far and near.
Have hearing health professionals (HHPs) acquired the same ability to prescribe, adjust, and meet the needs of the patients they/we serve? Consumer Reports14 recently suggested that, based on probe-microphone measures, 2 out of 3 hearing aids fit in the United States may be misfit, although we do not know the definition or degree of “misfit” from their report.
Given the variability in hearing aid fitting protocols—as well as unpredictable patient success with hearing aids, high return rates, 1-million-plus hearing aids in the drawer, lower-than-expected benefit achieved by the patient,14,26 and the inability to achieve brand loyalty with hearing aids—we believe it is important to explore the impact of the hearing healthcare process with a focus on the HHP’s role in improving patient success with hearing aids.
To do this, we will explore the relationship between aspects of the hearing healthcare protocol (“inputs”) and patient success (“outputs”). As in the previous publication,2 our focus will be on new hearing aids that are 4 years of age or less, fitted to both new and experienced hearing aid users:
- We compared new and experienced user experiences during the hearing aid fitting process.
- We compared protocols used for successful and unsuccessful hearing aid users and assessed their real-world success.
- We compared real-world success of hearing aid users receiving a “minimalist” protocol and those receiving a relatively “comprehensive” protocol.
Method
Detailed methodology for the MarkeTrak VIII survey is documented in detail in the first publication.2 To summarize, in November and December 2008, a short screening survey was mailed to 80,000 members of the National Family Opinion (NFO) panel as a means of identifying people with hearing loss and hearing aid owners. The NFO panel consists of households that are balanced to the latest US census information with respect to market size, age of household, size of household, and income within each of the 9 census regions, as well as by family versus non-family households, state (with the exception of Hawaii and Alaska), and the nation’s top 25 metropolitan statistical areas.
This short screening survey was completed by 46,843 households; 14,623 people with hearing loss were identified, and detailed demographics on those individuals and their households were obtained. The response rate to the screening survey was 59%. In January 2009, an extensive 7-page legal-size survey was sent to the total universe of hearing aid owners in the panel database (3,789); 3,174 completed surveys were returned, representing an 84% response rate.
In querying our MarkeTrak VIII database for hearing aids 4 years of age or less, we found 1,141 experienced users and 884 new users. The input variables and output variables are defined below. For the interested researcher or reader, we have documented the MarkeTrak survey on the Better Hearing Institute Web site (www.betterhearing.org).27
Input variables. The survey was designed in part to measure variables under control of the HHP that appear to be related to success with hearing aids including the following. However, one of the key variables we were unable to measure was quality control of the hearing aid, or “Did the HHP use a hearing aid analyzer and other methods to verify functionality of the hearing aid prior to the fit (eg, harmonic distortion, directional microphones wired correctly, noise cancelling circuit working, etc)?” This is something we could not ask the patient since they did not have knowledge of HHP practices prior to fitting the hearing aids.
However, the following variables were reported by the survey respondent/patient:
- Fit and comfort of the hearing aid as rated by the patient (1 survey item measured on a 7-point Likert scale).
- Achieved sound quality of the hearing aid as rated by the patient. One could, of course, argue that this is a shared responsibility of the manufacturer and the hearing healthcare professional. But it is our thesis that, with the sophistication of the hardware and software available, the HHP has at their disposal the ability to optimally amplify the residual auditory area, and that skill in this area contributes to the success or failure of the fitting. While we recognize that an independent assessment of the audiological fit of the hearing aid would be a better criterion, we used achieved sound quality as a proxy measure for optimal amplification of the residual auditory area, as well as performance of the hearing aid relative to specifications (eg, quality control of instrument prior to fit). The items chosen from the MarkeTrak survey database to measure achieved sound quality include: clearness of tone/sound, whistling and feedback, use in noisy situations, natural sounding, sound of voice, ability to hear soft sounds, and comfort with loud sounds (7 survey items, each measured on a 7-point Likert scale).
- Attributes of the HHP as rated by the patient, including knowledge, professionalism, empathy, creation of realistic expectations, explained care and maintenance of hearing aids, and quality of service during and after the fitting process (7 survey items, each measured on a 7-point Likert scale).
- Attributes of the HHP’s office as rated by the patient, including front office staff, hours of operation, attractiveness and comfort of the office, ease of access to the office, and convenient location (5 survey items, each measured on a 7-point Likert scale).
- Counseling or the amount of time (in hours) the HHP spent with the patient explaining care and maintenance of the hearing aids and the hours spent in auditory rehabilitation, as well as total counseling hours spent in the first 2 months of the new hearing aid fitting (numerical value in hours assigned by the patient).
- The number of visits required to achieve a desirable outcome from the patient’s perspective (numerical value assigned by the patient).
- Protocol steps received as perceived by the patient. An aided awareness survey was administered to each patient in which they indicated “Yes,” “No,” and “Not sure” to receiving the following 11 components of the hearing aid fitting protocol: hearing tested in sound booth, real ear measurement verification, subjective benefit measurement, objective benefit measurement (pre-post measurement of speech comprehension), patient satisfaction measurement, loudness discomfort measurement, auditory retraining software therapy, aural rehabilitation group, received self-help book, received self-help video, referred to self-help group (eg, HLAA). Great care was taken by an expert panel of audiologists to describe these aspects of the protocol in a language that could be understood by the patient.
|
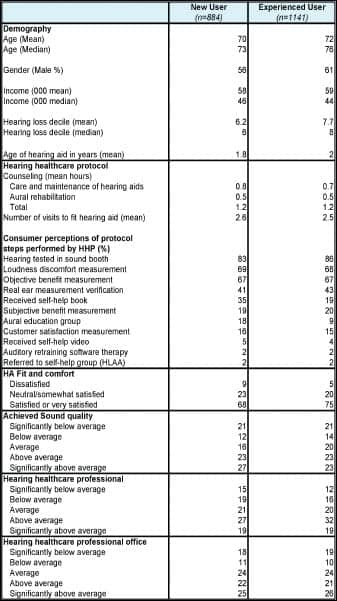
| TABLE 1. Hearing aid user characteristics and hearing healthcare process details. Click on image for larger view |
The variables of fit and comfort, sound quality, attributes of the HHP, and attributes of the HHP’s office were subjected to a factor analysis with Varimax rotation as a means of achieving four uncorrelated factor measures:
- Achieved sound quality
- HHP attributes
- HHP office attributes
- Fit and comfort
Uncorrelated factor scores for factors 1-3 were output and standardized to z scores with a mean of 5 and standard deviation of 2, creating normally distributed scores ranging from 1 to 9 (stanine scores). Since fit and comfort occupied its own factor space, the simple Likert scale rating was used in this analysis.
Output variables. There are many ways to measure patient success with hearing aids. The primary purpose of treating people with hearing loss with amplification is to do our very best job in compensating for their hearing loss while helping them to reclaim listening situations that are important to them. Without proper amplification one cannot achieve benefit; without substantial benefit, it is impossible for the HHP to impact positively the patient’s quality of life. The variables chosen for this analysis are as follows:
- Hearing aid usage (in hours) and hearing aids “in the drawer” (patient never uses the hearing aids).
- Benefit and satisfaction
- Patient satisfaction rating of the ability of their hearing aid to “improve their hearing” (7-point Likert scale)
- Perception of problem resolution or hearing handicap reduction in 10 listening situations. Patients were asked to estimate the percentage of hearing problems that were specifically resolved using their hearing aids. A factor analysis determined that there was only one factor in the ratings. Thus, this variable was calculated as the mean of the benefit achieved due to hearing aids in all 10 listening situations. Patients were asked to rate only those listening situations that were important to them.
- Multiple Environmental Listening Utility (MELU) or the percent of listening situations in which the patient was “satisfied” or “very satisfied.” Patients were asked to choose listening situations from a list of 19 that were important to them. The patient’s MELU rating is the percent of their list of listening situations in which they were satisfied or higher. Thus, one could view this as a quantified Client Oriented Scale of Improvement (COSI) measure.28
- Patient recommendations
- Would the patient recommend the HHP?
- Would the patient recommend hearing aids to friends?
- Would the patient repurchase their current hearing aid brand?
- Overall success. A composite measure of success was derived by factor analysis of the above variables, converting to factor scores and standardizing to a z score with a mean of 5 and standard deviation of 2 (stanine scores).
|
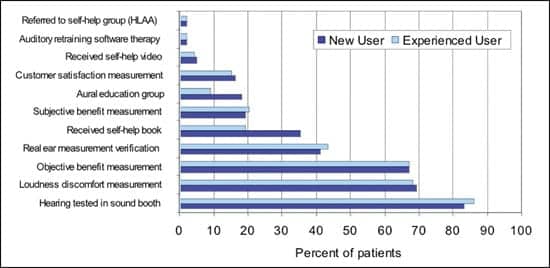
| FIGURE 1A. Perceptions of hearing aid fitting protocol received comparing new and experienced hearing aid users. |
|
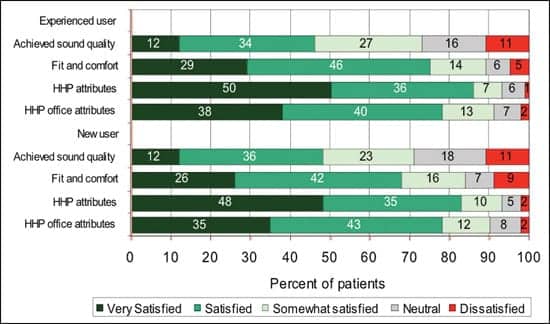
| FIGURE 1B. Patient perceptions of hearing aid fitting protocol received with a focus on patient satisfaction relative to overall sound quality of hearing aid (=4 years old), fit and comfort, and the hearing care provider and office attributes. Experienced users shown on top; new users shown on bottom. |

|
| FIGURE 2. Hearing aid usage comparing new and experienced users. |
|
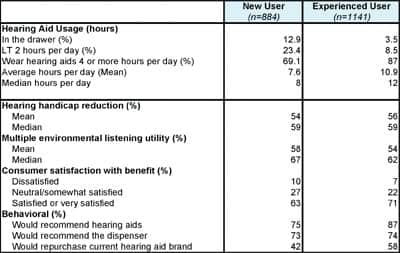
| TABLE 2. Hearing aid user outcome measures comparing new and experienced users (hearing aids <= 4 years of age). Click on image for larger view |
Results
New versus experienced users. Table 1 documents the characteristics of the sample and the protocol that was received by new and experienced users. The experienced users are slightly older by 2 years, have a greater proportion of male subjects (by 5 percentage points), and have more of a hearing handicap with a hearing loss decile of 7.7 compared to 6.2 for new users. (Note: Hearing loss deciles were derived based on composite measures of subjective hearing loss in the first publication in this series.2 A decile is calculated by simply dividing the hearing loss population into “buckets” of 10% each, where Decile 1 (bottom 10%) has very mild hearing loss and Decile 10 (top 10%) has a severe-to-profound hearing loss.)
Counseling and protocols observed by patients. On average, both groups (new and experienced users) received an average of 1.2 hours of counseling during the first 2 months of the hearing aid fitting process and required 2.5 visits (average) to fit their hearing aids.
Patients showed great discernment in indicating the presence or absence of 11 aspects of the fitting protocol. These are ranked from most prevalent to least prevalent in Table 1 and Figure 1a. The majority of users (83% new, 86% experienced) had their hearing tested in a sound booth. Approximately 7 out of 10 patients received a loudness discomfort measure, 2 of 3 were given objective benefit measures to verify the hearing aid fitting, but only 4 of 10 received real-ear measurement to verify the hearing aid fitting.
New users were more likely to receive a self-help book (35% versus 19%) and were more likely to attend an aural rehabilitation group (18% versus 9%). About 2 out of 10 patients were administered a subjective benefit measure, and 1 of 7 patients were administered a post-fitting patient satisfaction measurement. Only 5% (or less) received a self-help video or auditory retraining therapy, or were referred to a self-help group such as HLAA.
|
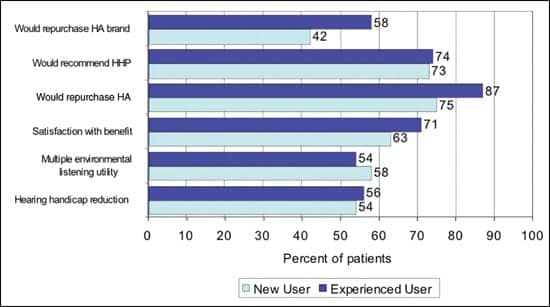
| FIGURE 3. Outcome measures for new and experienced users. |
Satisfaction and outcomes. As demonstrated in Figure 1b, experienced users were more satisfied with their hearing aid fit (75% versus 68%) while both groups were nearly equivalent on perception of sound quality achieved (mean of 7 items), ratings of the HHP’s attributes (mean of 7 items), and the attributes of the HHP’s office (mean of 5 items).
With respect to outcomes (Table 2 and Figure 2), nearly 13% of new users have their hearing aids in the drawer compared to 3.5% of experienced users; 1 in 4 new users use their hearing aids less than 2 hours a day. Experts generally agree that hearing aid users who wear their hearing aids at least 4 hours a day are considered potentially successful users. About 7 out of 10 new users wear their hearing aids 4 or more hours a day compared to nearly 9 of 10 experienced users.
Both new and experienced users report hearing aids have reduced their hearing handicap (Figure 3) by slightly more than 50%, and their hearing aids function effectively in 54% and 58%, respectively, of listening environments important to them. Experienced users are more satisfied with the achieved benefit (71% versus 63%) and are more likely to recommend hearing aids to their friends (87% versus 75%). Experienced users also have a greater likelihood of repurchasing their current brand of hearing aids when it is time to replace them (58% versus 42%). Approximately 3 of 4 new and experienced users would recommend the HHP who fit their hearing aids.
|
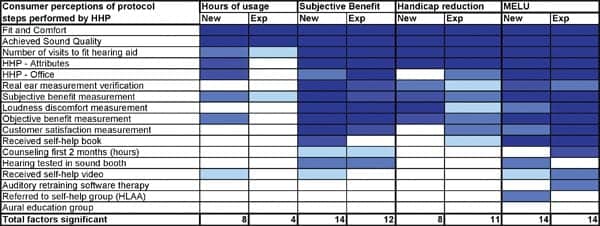
| TABLE 3A. The impact of the hearing care process on hours of hearing aid use, subjective benefit, handicap reduction, and multi-environmental utility, including comparisons between new and experienced users. The four shades of blue represent levels of statistical significance (darker shades = higher significance levels), as shown at bottom of Table 3B. |
|
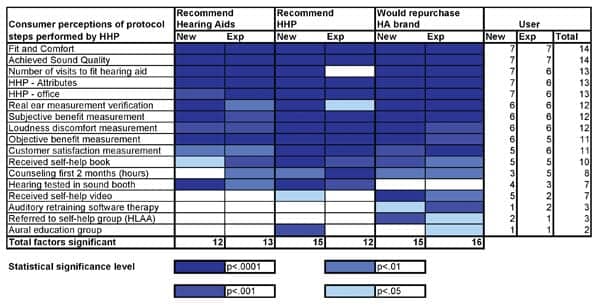
| TABLE 3B. The impact of the hearing care process on three measures of success: Would the new and experienced user 1) Recommend hearing aids; 2) Recommend the hearing healthcare practitioner, and 3) Recommend the same brand of hearing aid? The four shades of blue represent levels of statistical significance, with darker shades corresponding to higher significance levels. |
Protocols employed and resulting outcomes. Tables 3a-b summarize and rank (from high to low) statistically significant relationships between each of the 17 protocol steps with each of the 7 outcome measures for both new and experienced users. The darker the color of blue, the greater the level of statistical significance; blank cells indicate that the protocol item and outcome are not correlated.
Protocol items with the highest number of statistically significant relationships are:
- Fit and comfort and achieved sound quality (a proxy measure for optimal amplification of the residual auditory area and hearing aid functionality);
- Number of visits to fit the hearing aid (the lower the better);
- HHP attributes and HHP office attributes;
- REM verification;
- Subjective benefit measurement; and
- Loudness discomfort measurement.
Since so few patients received aural rehabilitation, were referred to a self-help group, or received auditory retraining therapy, at this time we cannot determine reliably the statistical significance of the relationship between these protocol items and real-world success.
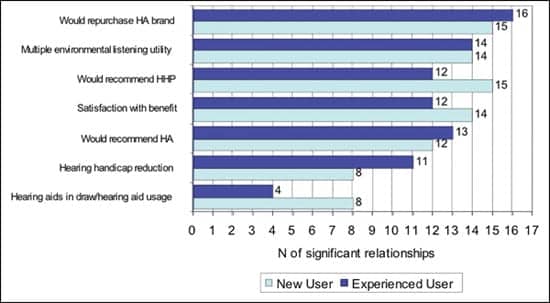
In Figure 4, the outcome measures most associated with the protocol are presented. Of the 7 outcome measures, the most highly correlated with the protocol is patient likeliness to repurchase the hearing aid brand (31 associations), followed by multiple environmental listening utility (28 associations), recommendation of the HHP (27 associations), and satisfaction with benefit (26 associations). Hours of usage and hearing aids in the drawer are least predictable from the protocol (4 associations for experienced users and 8 associations for new users).
In the final analysis, we have pooled new and experienced users because their overall protocols were statistically equivalent.
|
| FIGURE 4. Overall summary of statistically significant relationships between outcome measures and protocol items comparing new and experienced hearing aid users (ie, the data in Tables 3a-b). The outcome variables are ranked based on total number of significant relationships. |
Relating the Protocol Received to a Total Measure of Success
To derive a total measure of success, a factor analysis was conducted on the seven outcome measures, resulting in a single index that was standardized to a mean of 5 and standard deviation of 2. The resulting sample size was 1,613 hearing aid users with total success scores. However, first the number of items in the protocol was reduced by five (from 17 to 12 items) by collapsing counseling methods used, taking the values “none” to “three or more.” The counseling methods were: aural rehabilitation group, referral to self-help group such as HLAA, received self-help book, received self-help video, and received auditory retraining therapy.
In Table 4, three high-low comparisons are documented: above- and below-average hearing aid success, top- and bottom-weighted protocols, and a minimum (min) and comprehensive (max) protocol. In the final three columns of this table are the difference scores between the high and low groups. Group descriptions are provided. At the bottom—shaded in green—are the individual outcome measures. Each of the high-low analyses will be discussed in sequence.
Above-average success vs below-average success with hearing aids. In comparing above-average and below-average hearing aid user success, individuals were compared who were at least one standard deviation below the mean (n=331) on success and those who were at least one standard deviation above the mean on success (n=407). The analysis was performed to answer the question: “Are there differences in the protocols observed for these two samples?” The difference scores are shown in the first column of the final three columns labeled “Success” in Table 4. These differences are also graphically portrayed in Figures 5a-e.
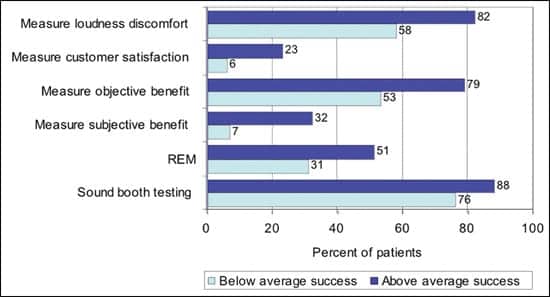
Hearing aid users with above-average success were most likely to receive objective benefit measurement (+26%), subjective benefit measurement (+25%), loudness discomfort measurement (+24%), real-ear measurement (+20%), and a patient satisfaction measurement (+17%), and to be tested in a sound booth (+12%).
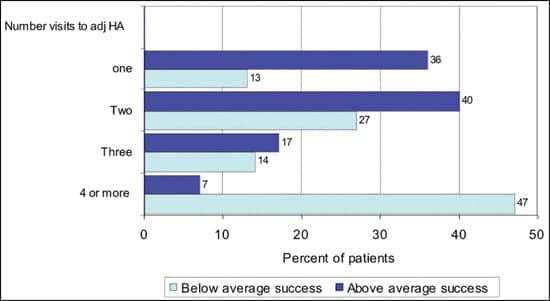
Office visits. One of the strongest relationships was the number of visits to fit the hearing aids (Figure 5b). Hearing aid users with above-average success were more likely to have their hearing aid fit in 1 or 2 visits (76%) compared to users with below-average success (40%). Interestingly, almost half of the below-average patients had 4 or more visits. As shown in Figure 5c, below-average patients were less likely to receive personal counseling from the hearing health professional (37% versus 22% for above-average patients) or ancillary counseling tools, such as auditory retraining software, self-help material, or referral to a self-help group (47% versus 36% for above-average patients).
Office attributes and HHP traits. Figure 5d graphs HHP and office attributes for the two success groups. Hearing aid users who are most successful show a greater likelihood of rating the HHP above average (+30) but not necessarily significantly above average (-4). This is a consistent finding across all the sub-analyses, as well as the total analysis.
In deriving uncorrelated factors in the protocol, the personality and likability of the HHP was effectively removed from the performance of the hearing aids (achieved sound quality). There is a small segment of HHPs with very favorable personalities, yet who were unable to provide hearing aid success. Above-average users were also more likely to rate the office attributes as above average to significantly above average (65%) compared to patients who were below average (37%).
Fit & comfort and sound quality. Figure 5e reports hearing aid fit and comfort and achieved sound quality. The above-average success group is more likely to be satisfied or very satisfied with their hearing aid fit and comfort (99% versus 63%) and have achieved above-average to significantly above-average sound quality (88% versus 12%); 55% of the below-average success group rate their achieved sound quality at least 2 standard deviations below the mean.
|
||||||
| FIGURE 5A. Six tests/measurements: A comparison of above-average (+1 std) and below-average (-1 std) hearing aid success as measured by subjective real-world outcomes showing protocol received based on patient perceptions. | ||||||
|
||||||
| FIGURE 5B. Number of patient visits to the practice: A comparison of above-average (+1 std) and below-average (-1 std) hearing aid success. | 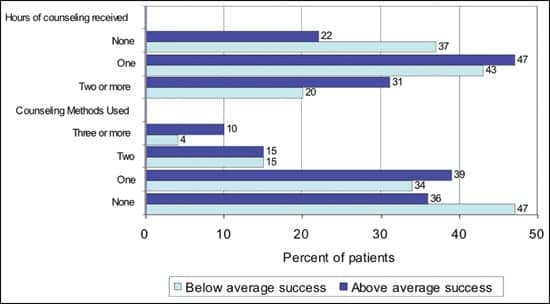
|
FIGURE 5C. Hours of counseling and the number of methods used: A comparison of above-average (+1 std) and below-average (-1 std) hearing aid success as measured by subjective real-world outcomes based on patient perceptions. | 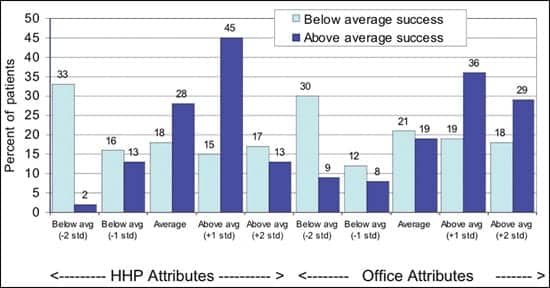
|
FIGURE 5D. HHP and HHP office attributes: A comparison of above-average (+1 std) and below-average (-1 std) hearing aid success as measured by subjective real-world outcomes based on patient perceptions. | 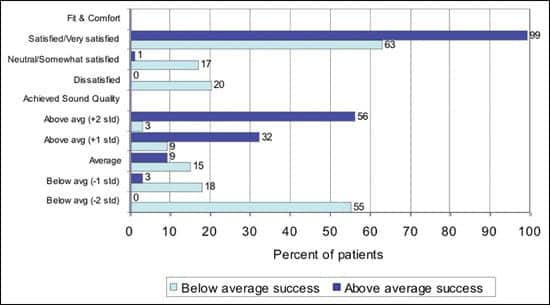
|
FIGURE 5E. Fit and comfort issues and achieved sound quality: A comparison of above-average (+1 std) and below-average (-1 std) hearing aid success as measured by subjective real-world outcomes based on patient perceptions. |
Comparing Success Based on Protocol Received
Do steps performed during the hearing aid fitting have an additive or multiplicative impact on real-world success? To address this issue, we performed two high-low analyses (n=1,850). In the first analysis, we simply took the difference scores (shown under success) and weighted the protocol based on these difference scores. This technique is used in the field of industrial psychology to compare employees who fail and employees who succeed, leading to predictive measures of success in the selection process.
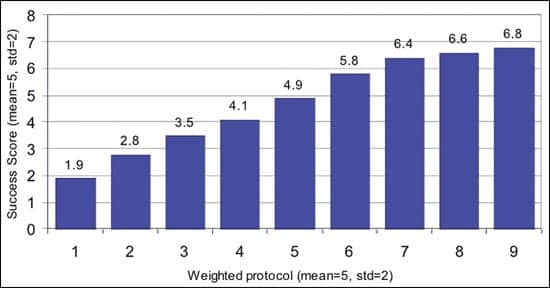
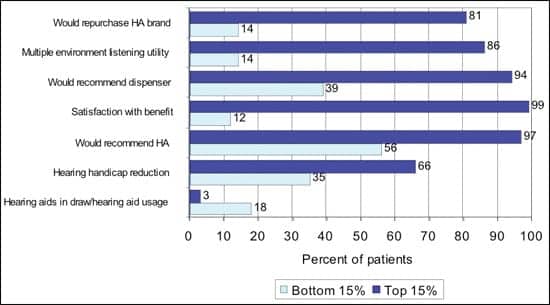
The range in weighted protocol scores was more than 465 points. Converting the weighted protocol to stanines (z scores with a mean=5, std=2), the mean success scores are plotted in Figure 6a. The overall correlation between the total success score and weighted protocol is 0.70 (p<.0001). We then took the top (n=275) and bottom (n=276) 15% of patients based on protocol scores and graphed their real-world success scores on the 7 outcome measures in Figure 6b with documentation in Table 4 under “Weighted protocol.”
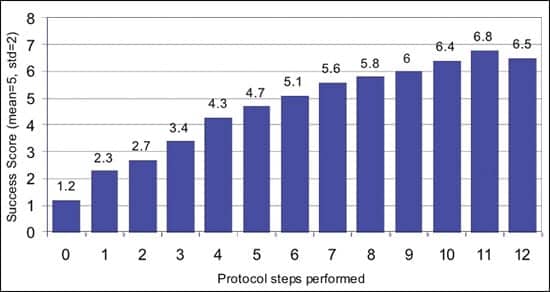
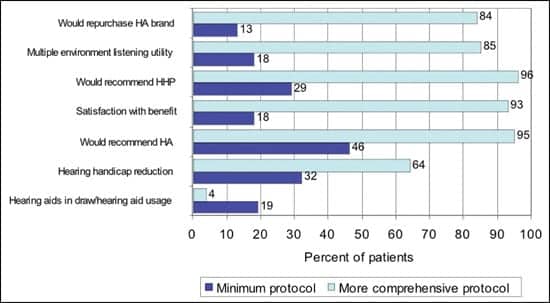
In the second analysis, we ranked patients on the number of items (range 0-12) or steps received during the hearing aid fitting process. The average total success scores are plotted by the number of protocol steps performed in Figure 7a, and the overall correlation is 0.52 (p<.0001). In Figure 6b and documented in Table 4 under “Unweighted protocol,” the outcomes of subjects receiving a minimalist protocol (“Min” 0-2, n=114) are compared to those receiving a more comprehensive protocol (“Max” 10-12, n=116).
|
| FIGURE 6A. Total hearing aid user success achieved as a function of a weighted fitting protocol (in stanines, n=1,613). |
|
| FIGURE 6B. Impact of a weighted protocol comparing the top and bottom 15% of patients on hearing aid success. |
Discussion
Both methods of relating the protocol to real-world success are comparable and demonstrate there are substantial differences in success (the output) based on the input (what occurred during the hearing aid fitting process).
The data strongly suggest that comprehensive protocols have a major impact on:
- Hearing aid brand loyalty;
- Utility of hearing aids;
- Positive-word-of mouth advertising;
- Satisfaction with benefit achieved;
- Hearing handicap reduction; and
- Hearing aid usage and reduction of hearing aids in the drawer
In addition, the data suggest that a weighted protocol may be more predictive of real-world success than simply counting the steps performed by the HHP.
Finally, we looked at other factors that might have influenced the protocol used. Age of the patient, gender, user (new versus experienced), size of city (rural to metropolitan), price of hearing aid, style of hearing aid, and degree of hearing loss explained less than 1% of variance in the protocol used.
In this study, 69% of hearing aids were fit by audiologists and 31% by hearing instrument specialists. The occupation of the hearing aid fitter explained less than one-half of 1% of the protocol used or hearing aid user real-world success.
|
| FIGURE 7A. Total hearing aid user success achieved as a function of an additive hearing aid fitting protocol (n=1,613). |
|
| FIGURE 7B. Impact of a protocol on hearing aid success comparing a minimum protocol (0-2 items) to a more comprehensive protocol (10-12 items). |
Critique of This Study and Suggestions for Further Research
Because of the method used (ie, mail survey), the inputs (protocol) and the outputs (measures of success) were simultaneously collected. Great care was taken in defining the inputs, and it is recognized (especially given the age group of the users) there could be errors in their perceptions of what occurred and what did not occur when they had their hearing aids fit. However, recall that there was discernment in patient evaluations of what occurred with a range of 2%-85%. There was no evidence of positive response bias for successful patients. Some of the data approximates reports from surveys of HHP offices across the United States (eg, relatively high likelihood of being tested in a sound booth, modest likelihood of benefit measure, low likelihood of REM, and very low likelihood of aural rehabilitation counseling).6,21
We hope this field survey, which is correlational in nature, facilitates a better field research model. Since the distribution of protocols performed and the distribution of patient success are so large across the United States, we believe that the clinical laboratory is the “real world.” Further, it seems reasonable that we can obtain an improved understanding of the quantity and quality of misfit hearing aids, as well as the relative importance of various aspects of the protocol. Although this type of study would be man-power intensive and expensive, it is critical to understand how inputs in the hearing aid fitting process impact real-world success.
Small-scale studies with sample sizes of 15-25, which vary one or more protocol variables, are not powerful enough statistically to advance the science of hearing aid fitting. As history has shown, these studies do not appear to prompt the HHP to change their behavior away from their traditional or most comfortable protocol.
Acknowledgements
This study was made possible by a special grant from Knowles Electronics LLC, Itasca, Ill. The authors wish to thank the following for their review and valuable comments in the preparation of this article: Harvey B. Abrams, PhD, Bay Pines VA Healthcare System, Bay Pines, Fla; Ruth Bentler, PhD, University of Iowa, Iowa City; Vic S. Gladstone, PhD, American Speech-Language-Hearing Association (ASHA), Rockville, Md; Larry E. Humes, PhD, Indiana University Bloomington; and Michael Valente, PhD, Washington University School of Medicine, St Louis.
References
- Kochkin S. MarkeTrak VIII: Customer satisfaction with hearing aids is slowly increasing. Hear Jour. 2010;63(1):11-19.
- Kochkin S. MarkeTrak VIII: 25-year trends in the hearing health market. Hearing Review. 2009;16(11):12-31.
- Kochkin S. MarkeTrak V: Why my hearing aids are in the drawer: The consumer’s perspective. Hear Jour. 2000;53(2):34-42.
- Kochkin S. MarkeTrak VII: Obstacles to adult non-user adoption of hearing aids. Hear Jour. 2007;60(4):27-43.
- Hearing Industries Association (HIA). Statistical reporting program. Washington, DC: 2010.
- Strom K. The HR 2006 dispenser survey. Hearing Review. 2006;13(6):16-39.
- Valente M. Guideline for audiologic management of the adult patient. Available at: www.audiologyonline.com/articles/article_detail.asp?article_id=1716. Accessed March 9, 2010.
- Valente M. Audiological management of adult hearing impairment. Audiology Today. 2006;18(5):32-36.
- American Speech Language Hearing Association (ASHA). Guidelines for Hearing Aid Fitting for Adults, ASHA Ad Hoc Committee on Hearing Aid Selection and Fitting. Available at: www.asha.org/docs/html/GL1998-00012.html. Accessed March 9, 2010.
- International Hearing Society (IHS). A Professional Practice Profile for Hearing Health Professionals. Available at: ihsinfo.org/IhsV2/Communities_Members/Professional_Practice_Profile.cfm. Accessed March 9, 2010.
- Purchasing a hearing aid: a patient checklist, Hearing Loss Association of America, Bethesda, Md. Available at: www.hearingloss.org/LEARN/docs/HLAAHearingAidChecklist_4-14-2009.pdf. Accessed March 9, 2010.
- Rogin C. Top 10 reasons for consumer delight. Washington, DC: Hearing Industries Association; 2010.
- US Food and Drug Administration (FDA). Guide to Hearing Aids. Washington, DC: FDA. Available at: www.fda.gov/MedicalDevices/ProductsandMedicalProcedures Home HealthandPatient/PatientProducts Hearing Aids/default.htm. Accessed March 9, 2010.
- Hear well in a noisy world. Consumer Reports. July 2009:32-37. http://www.consumerreports.org.
- Christensen L, Groth J. Top ten clinician mistakes in geriatric hearing aid fitting. Seminar presented at: American Academy of Audiology; April 2008; Dallas.
- Aarts N, Cafee C. Manufacturer predicted and measured REAR values in adult hearing aid fitting: accuracy and clinical usefulness. Int J Audiol. 2005;44:293-301.
- Aazh H, Moore BC. The value of routine real ear measurement of the gain of digital hearing aids. J Am Acad Audiol. 2007;18:653-664.
- Bentler R. Advanced hearing aid features: do they work? Seminar presented at: American Speech Language Hearing Association annual convention; 2004; Washington, DC.
- Hawkins D, Cook J. Hearing aid software predictive gain values: how accurate are they? Hear Jour. 2003;56(7):26-34.
- Beck DL. Do real-ear measurements make a real difference to patient outcomes? Available at: www.audiology.org/news/interviews/Pages/20090119a.aspx. Accessed March 9, 2010.
- Kirkwood D. Survey: Dispensers fitted more hearing aids in 2005 at higher prices. Hear Jour. 2006;59(4):40-50.
- Yanz JL, Pisa JFD, Olson L. Integrated REM: real-ear measurement from a hearing aid. Hearing Review. 2007;14(5):44.51.
- Mueller GH. Probe-mic measures: hearing aid fitting’s most neglected element. Hear Jour. 2005;58(10):21-30.
- Cunningham DR, Williams KJ, Goldstein LJ. Effects of providing and withholding post-fitting fine-tuning adjustments on outcome measures in novice hearing aid users: a pilot study. Am J Audiol. 2001;10:51-65.
- Shi L, Doherty K, Kordas T, Pellegrino J. Short-term and long-term hearing aid benefit and user satisfaction: a comparison between two fitting protocols. J Am Acad Audiol. 2007;18:482-495.
- Kochkin S. MarkeTrak VI: On the issue of value: hearing aid benefit, price, satisfaction and brand repurchase rates. Hearing Review. 2003;10(2):12-25.
- Kochkin S. MarkeTrak VIII survey. Available at: www.betterhearing.org/professionals/tools.cfm [under Instruments]. Accessed March 9, 2010.
- Dillon H, James A, Ginis J. Client oriented scale of improvement (COSI) and its relationship to several other measures of benefit and satisfaction provided by hearing aids. J Am Acad Audiol. 1997;8:27-43.
Correspondence can be addressed to HR or Sergei Kochkin, PhD, at.
Citation for this article:
Kochkin S, Beck DL, Christensen LA, Compton-Conley C, Kricos PB, Fligor BJ, McSpaden JB, Mueller HG, Nilsson MJ, Northern JL, Powers TA, Sweetow RW, Taylor B, Turner RG. MarkeTrak VIII: The impact of the hearing healthcare professional on hearing aid user success. Hearing Review. 2010;17(4):12-34.