Research | April 2014 Hearing Review
The biggest obstacle for those with mild losses may be the clinicians themselves.

Did you know that adult-onset hearing loss is recognized by the World Health Organization (WHO) as the third leading cause of disability, with a mild impairment being the most prevalent? The WHO estimated in 2012 that, in regions such as North America, Western Europe, and Australasia, 1 in 3 adults over 65 years old have a mild hearing loss.
Combining this prevalence estimate with the WHO prediction that the number of adults over 65 years old will triple between 2010 and 2050, it can be seen that mild hearing impairment will increasingly affect older adults in the future.
How Common Is Mild Hearing Loss?
The prevalence rate of mild hearing loss is strongly dependent on how this degree of hearing loss is defined. The WHO prevalence statistics from 2012 were based on a definition of mild hearing loss being an average threshold at 500, 1000, 2000 and 4000 Hz of between 26 and 40 dB HL, and calculated mild hearing loss for all adults 15 years or older to be 9% to 17%, depending on geographic region.1 In another WHO review in 2013, by the Global Burden of Disease Hearing Loss Expert, the global prevalence rate was 22.7% for men and 19.0% for women for adults over age 15. That study defined mild hearing impairment as thresholds between 20 and 34 dB HL (averaged over 0.5, 1, 2, and 4 kHz) and pointed out the prevalence of hearing loss rises sharply for adults over the age 50.2
The effect that the definition and sample group age can have on prevalence rates was also documented by a Finnish population study in 1997. Uimonen et al3 sampled a general population group of adults between 55 and 75 years old and, using a definition of mild hearing impairment being a four frequency hearing loss (4FAHL) at 500, 1000, 2000, and 4000 Hz between 21-39 dB, showed the prevalence rate was 29.5%. This was significantly higher than the prevalence rate in the same population group of 10.1% when using a 3FAHL at 500, 1000, and 2000 between 26-40 dB HL.
This is in line with Australian population-based studies, such as the Blue Mountains Study, which also used the same 4FAHL but a threshold range of 25 to 40 dB HL, and reported a mild hearing impairment prevalence of 39.1% in adults over age 55 years.4
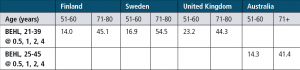
Table 1 shows the prevalence rates and definitions used by a number of other European and Australian studies. All studies used the average hearing loss in the better ear, or BEHL.
From these studies, the conclusion can be reached that, by age 71 and older, close to 1 in 2 adults have a mild hearing impairment.5,6
 What Is the Impact of a Mild Hearing Loss?
What Is the Impact of a Mild Hearing Loss?
The literature confirms what many clinicians regularly observe in their clinics; for some clients, even a mild or marginal hearing impairment can result in less satisfaction with own independence, reduced emotional well-being, and greater perceived limitation.7-11 Other clients may show similar audiometric results, yet report no problems or limitations.
Some studies suggest that setting a minimum pure-tone threshold average at which a hearing loss could be deemed to be disabling may not be valid.12,13 Lutman and his group concluded that for some individuals an average loss of 15 dB HL was significantly disabling for everyday speech.12
As pure-tone thresholds measure hearing sensitivity but not communication ability, speech audiometry is often used as a clinical tool to assess a client’s speech intelligibility using materials and presentation levels that better represent everyday speech. But, in the case of mild hearing loss, is speech audiometry more closely related to hearing difficulty?
Unfortunately, the answer remains unclear. A number of studies have investigated the relationship between pure-tone thresholds, various speech audiometry results, and self-reported hearing difficulty. Many of these studies have two conclusions in common:
1) The reported correlations are often significant, but only mild or moderate in scale, and
2) Individual variability in speech scores is large among participants with mild hearing impairment.14-19
Overall, it was found that speech performance could not be predicted by pure-tone thresholds, and speech-in-noise results could not be predicted by speech in quiet measures.
For example, Duquesnoy15 investigated speech intelligibility in 110 adults between ages 60 and 90—all of whom had a 3FAHL less than 50 dB HL and 88% below 40 dB HL. He found participants with similar speech scores in quiet showed large variability in speech-in-noise tests, and concluded one could not be predicted from the other. This highlights the clinical relevance of testing both in quiet and in noise, although the Duquesnoy study did not address any age effects that could be expected in a sample of older adults. In a follow-up to his 1987 study, Lutman20 demonstrated that older adults with mild hearing impairment showed worse speech measures performance, but reported less disability, than younger adults. Once the effects of age and degree of hearing impairment were averaged out, there was no correlation between speech-in-noise measures, speech in quiet, and self-reported disability.
Possible age-related effects also were addressed by Dubno et al16 who measured speech recognition in quiet and in noise, in 72 younger and older adults with either normal hearing or a mild hearing loss. Her study showed that age was not a contributing factor when measuring speech understanding in quiet and that, particularly for sentences with low predictability, participants with mild hearing loss showed significant differences compared to normal-hearing participants. For speech in noise understanding, the participant’s hearing loss, age, the speech material used, and the level of presentation of the speech all played a significant role.
Divenyi and Haupt21 also addressed the complexity of the relationship between age and hearing loss and point out that different speech understanding tasks can be affected by either peripheral hearing loss or age, or both.
In all, the relationship of speech audiometry results and everyday hearing difficulties for older individuals with a mild hearing loss is complex.
The Strength of Self-report
It seems increasingly clear that everyday hearing difficulties cannot be predicted from standard audiometric testing, and that the true measure of hearing loss lies in the client’s report of how they experience their hearing.
One self-report measure often used in the scientific literature is the Hearing Handicap Inventory for the Elderly (HHIE), which has been deemed to be a valid and robust measure of the emotional and social effects of hearing impairment.22 Weinstein and Ventry23 reported that the greatest degree of variability in the self-report scores was for participants with a 3FAHL of 26-40 dB HL in the better ear, with some reporting significant disability and others none at all. They also concluded that speech recognition in quiet scores accounted for less than 20% of variance in HHIE scores—again underpinning the notion that speech audiometry does not truly reflect everyday hearing difficulties.
Others found the correlations between the HHIE and speech-in-noise tests were similarly low. Matthews et al14 demonstrated that SPIN results were no better correlated with HHIE scores than, for example, pure-tone thresholds at 1000 and 2000 Hz.
The concluding message from these studies must be that there is not one true measure of hearing disability for clients with mild hearing loss, and that as clinicians we are best guided by obtaining as comprehensive a picture of our clients’ hearing difficulties as possible. The best indication of how your client is experiencing their hearing loss may not lie in standard clinical tests but in what they tell us about their activities and participation. One large-scale review of the literature by Knudsen et al,24 looking at help-seeking for hearing loss and hearing aid outcomes, concluded that self-reported activity limitation, or disability, was the one factor that emerged as highly important in all aspects of aural rehabilitation, more so than measured hearing loss.
Are We Meeting the Challenge?
The most common aural rehabilitation approaches for adult-onset hearing loss today are the provision of hearing aids. However, a number of consumer studies have suggested that, among other barriers, one influencing factor for lower adoption of hearing aids for those with mild hearing loss may be the clinicians themselves.
The MarkeTrak series of consumer questionnaires tracks attitudes and trends among individuals with hearing loss and the hearing aid market in the United States. The MarkeTrak survey in 2012 suggested that 29% of individuals who report a mild hearing loss had discussed their hearing problems with an audiologist and 43% were advised to wait and retest, while 26% were told that hearing aids would not be beneficial.25 The European equivalent of MarkeTrak is EuroTrak, which monitors six European markets including the United Kingdom. The UK EuroTrak 2012 results showed that 19% of respondents who reported a hearing problem and did not own a hearing aid had discussed their hearing with either a hearing aid dispenser or audiologist and 51% of these were recommended not to get a hearing aid.26
While these consumer studies cannot comment on whether the individuals were appropriate hearing aid candidates, or if their recollection of the advice given was accurate, the numbers reporting that hearing aids were not (yet) recommended are significant. One reason for advising against hearing aids may be that hearing aids are deemed less beneficial for those with mild hearing loss, although some studies have shown this not to be the case.27,28 The results presented by Davis et al27 showed that benefit with hearing aids was not significantly better for those with a 4FAHL in the worse ear of 30-39 dB HL than for greater losses, although benefit for participants with a 4FAHL of 25-29 dB HL was significantly less. The study did show that use of hearing aids increased with increasing degrees of hearing loss but was careful to point out that dimension, such as benefit and satisfaction, did not show such clear correlation with average thresholds. Therefore, it is important to recognize that measuring use is not the same as measuring benefit, and vice versa.
In investigating hearing aid outcomes for clients with mild hearing loss, Dillon28 presented that composite benefit (a dimension that includes self-reported benefit, use, satisfaction, and quality of life) was not significantly correlated with the 4FAHL in the better ear but was better determined by the individual’s need for hearing aids. As Dillon pointed out, the dimension of need can be defined as unaided hearing difficulties and a desire or motivation toward hearing aids.
Self-reported hearing difficulties and attitude toward hearing aids, as well as the support of significant others (and the hearing aid’s insertion gain), were also shown by Hickson and Meyer29 to be variables that showed differences between successful and unsuccessful hearing aid wearers.
Toward Successful Outcomes for Mild Hearing Loss
In all, the conclusion can be reached that there is a significant group of individuals with mild hearing loss who do experience reduced speech understanding in everyday listening situations. Some of these people visit clinics and dispensing offices to discuss their hearing difficulties with hearing care professionals. If these clients demonstrate a positive attitude to hearing aids, there is no reason to suggest that their benefit from amplification will be any less than those with greater hearing loss.
The concluding message from these studies must be that there is not one true measure of hearing disability for clients with mild hearing loss, and that as clinicians we are best guided by obtaining as comprehensive a picture of our clients’ hearing difficulties as possible.
References
1. World Health Organization. WHO global estimates on prevalence of hearing loss. Geneva: World Health Organization; 2012.
2. Stevens G, Flaxman S, Brunskill E, et al. Global and regional hearing impairment prevalence: an analysis of 42 studies in 29 countries. Eur J Public Health. 2013;23(1):146-52.
3. Uimonen S, Mäki-Torkko E, Jounio-Ervasti K, Sorri M. Hearing in 55 to 75 year old population in northern Finland—a comparision of two classifications of hearing impairment. Acta Otolaryngol Suppl. 1997;529:69-70.
4. Sindhusake D, Mitchell P, Smith W, et al. Validation of self-reported hearing loss: the Blue Mountains Hearing Study. Int J Epidemiol. 2001;30(6):1371-8.
5. Shield B. Evaluation of the social and economic costs of hearing impairment: Hear-it; 2006. Available at: http://www.political.hear-it.org/multimedia/Hear_It_Report_October_2006.pdf
6. Wilson DH, Walsh PG, Sanchez L, et al. The epidemiology of hearing impairment in an Australian adult population. Int J Epidemiol. 1999;28:247–52.
7. Scherer MJ, Frisina R. Characteristics associated with marginal hearing loss and subjective well-being among a sample of older adults. J Rehabil Res Dev. 1998;35:420-6.
8. Monzani D, Galeazzi GM, Genovese E, Marrara A, Martini A. Psychological profile and social behaviour of working adults with mild or moderate hearing loss. Acta Otorhinolaryngol Ital. 2008;28(2):61-6.
9. Bertoli S, Bodmer D, Probst R. Survey on hearing aid outcome in Switzerland: associations with type of fitting (bilateral/unilateral), level of hearing aid signal processing, and hearing loss. Int J Audiol. 2010;49(5):333-46.
10. Suter AH. The ability of mildly hearing-impaired individuals to discriminate speech in noise. Washington, DC: US Environmental Protection Agency; 1978.
11. van Boxtel MPJ, van Beijsterveldt CEM, Houx PJ, Anteunis LJC, Metsemakers JFM, Jolles J. Mild hearing impairment can reduce verbal memory performance in a healthy adult population. J Clin Exp Neuropsychol. 2000;22:147-54.
12. Lutman M, Brown EJ, Coles RRA. Self-reported disability and handicap in the population in relation to pure-tone threshold, age, sex and type of hearing loss. Br J Audiol. 1987;21(1):45-58.
13. Bess FH, Lichtenstein MJ, Logan SA. Making hearing impairment functionally relevant: Linkages with hearing disability and handicap. Acta Otolaryngol Suppl. 1990;476:226-31.
14. Matthews LJ, Lee F-S, Mills JH, Schum DJ. Audiometric and subjective assessment of hearing handicap. Arch Otolaryngol Head Neck Surg. 1990;116(11):1325 – 30.
15. Duquesnoy AJ. The intelligibility of sentences in quiet and in noise in aged listeners. J Acoust Soc Am. 1983;74(4):1136-44.
16. Dubno JR, Dirks DD, Morgan DE. Effects of age and mild hearing loss on speech recognition in noise. J Acoust Soc Am. 1984;76(1):87-96.
17. Tyler S, Smith PA. Sentence identification in noise and hearing-handicap questionnaires. Scand Audiol. 1983;12:285-92.
18. Smoorenburg GF. Speech reception in quiet and in noisy conditions by individuals with noise-induced hearing loss in relation to their tone audiogram. J Acoust Soc Am. 1992;91(1):421-37.
19. Helfer KS, Freyman RL. Aging and speech-on-speech masking. Ear Hear. 2008;29(1):87-98.
20. Lutman M. Hearing disability in the elderly. Acta Otolaryngol Suppl. 1990;476:239-48.
21. Divenyi P, Haupt K. Audiological correlates of speech understanding deficits in elderly listeners with mild-to-moderate hearing loss. I. Age and lateral asymmetry. Ear Hear. 1997;18(1):42-61.
22. Ventry I, Weinstein B. The Hearing Handicap Inventory for the Elderly: a new tool. Ear Hear. 1982;3(3):128-34.
23. Weinstein BE, Ventry IM. Audiometric correlates of the Hearing Handicap Inventory for the Elderly. J Speech Hear Disord. 1983;48(4):379-84.
24. Knudsen LV, Oberg M, Nielsen C, Naylor G, Kramer SE. Factors influencing help seeking, hearing aid uptake, hearing aid use and satisfaction with hearing aids: a review of the literature. Trends Amplif. 2010;14(3):127-54.
25. Kochkin S. MarkeTrak VIII: The key influencing factors in hearing aid purchase intent. Hearing Review. 2012;19(3):12-25. Available at: https://hearingreview.com/2012/03/marketrak-viii-the-key-influencing-factors-in-hearing-aid-purchase-intent
26. EHIMA. EuroTrak 2012. 2012 [cited February 23, 2013]. http://www.ehima.com/ehima2/
27. Davis A, Smith P, Ferguson M, Stephens D, Gianopoulos I. Acceptability, benefit and costs of early screening for hearing disability: a study of potential screening tests and models. Health Technol Assess. 2007;11(42):1-294.
28. Dillon H. Hearing Loss: The Silent Epidemic. 17th National Conference of the Audiological Society of Australia. Perth, Australia; 2006.
29. Hickson L, Meyer C, Lovelock K, Lampert M, Khan A. An investigation of factors that influence help-seeking for hearing impairment in older adults. Intl J Audiol; 2014:1-15.
About the author: Barbra Timmer, MACAud, MAudSA, MBA, completed her Audiology studies at the University of Queensland in Australia, and her MBA from the Sydney Graduate School of Management. After holding several clinical positions in Australia and Europe, she joined Phonak in 1996 and transferred to its headquarters in Switzerland in 2003, eventually serving as the company’s Director of Audiology and Education. Timmer recently returned to Australia and started a research degree at the University of Queensland, supported by a studentship from Phonak AG. C
Correspondence can be addressed to: [email protected]
Original citation for this article: Timmer B. It may be mild, slight, or minimal, but it’s not insignificant. Hearing Review. 2014;21(4):30-33.