Tech Topic | November 2016 Hearing Review
Our professional future involves customized hearing healthcare. And the future is bright.
The time is ripe for audiologists and hearing care professionals to consider new strategies to achieve the two goals of providing quality hearing healthcare and ensuring profitability for the hearing healthcare practice. The ground is shifting precipitously, with changing government rules and regulations, new technologies such as personal sound amplification products (PSAPs), automated hearing tests, and inexpensive hearing aids offered by Big Box retailers.1,2 Our clientele is increasingly asking the question, “Why should I go to an audiologist when I can get a hearing test at the drug store and I can buy a good hearing aid at Costco?” And, increasingly, our typical answers—I have a professional degree; I can give you a better listening device; I know how to test the hearing of a difficult-to-test patient—seem less compelling to savvy consumers who are interested in maximizing the dollars they spend on healthcare.
-Only about 20% of new hearing-aid users receive aural rehabilitation beyond hearing aids.3
-Only about 10% of experienced hearing aid users receive aural rehabilitation beyond hearing aids.3
-New hearing aid users on average receive less than a half hour of counseling.3
-Only about 5% of new hearing aid users are provided with formal re-training opportunities.3
-If patients are just beginning the hearing healthcare journey and are not yet interested in purchasing hearing aids, the audiologist typically focuses on creating motivation to purchase hearing aids rather than offering alternative treatments to help them start their journey.4
Table 1. Evidence that most hearing care professionals do not provide aural rehabilitation other than hearing aids.
When considering the facts in Table 1, most readers would agree that, for many audiological practices, selling hearing aids comprises the bulk of what audiologists and hearing care professionals consider for hearing treatment. While this isn’t necessarily a “bad” strategy—after all, people with hearing loss do benefit greatly from receiving well-fitted hearing aids—in this day and age, it is most assuredly a shortsighted strategy because it does not take into account current market forces.
Game-based Learning and Customized Hearing Healthcare
Any new strategy for providing quality hearing healthcare should incorporate two fundamental components:
1) Customization that allows quality hearing healthcare superior to what is made available through other channels, and
2) Maximum use of the Internet, which allows practices to sustain profitability.
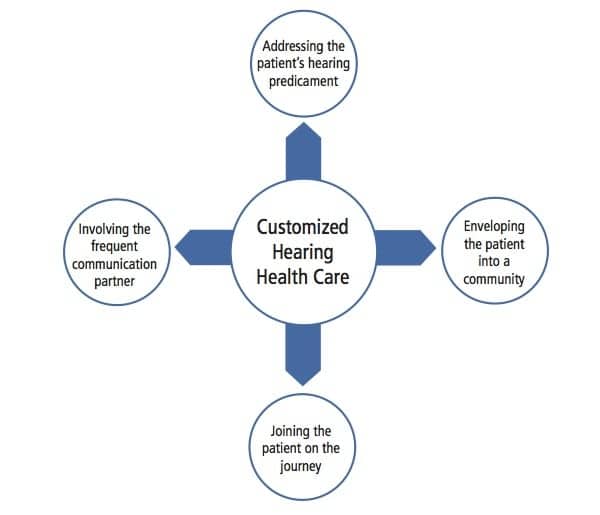
Figure 1. A model for customized hearing healthcare. The model is comprised of four key components for ensuring quality hearing healthcare.
Figure 1 presents the model for this customized hearing healthcare strategy. It is comprised of four key elements:
1) Understanding and addressing the patient’s hearing predicament;
2) Including the patient’s frequent communication partner(s) in the hearing treatment plan;
3) Creating a sense of community with others who share similar hearing-related concerns and challenges; and
4) Making the hearing care professional a fellow traveler in the patient’s journey of navigating the world with a hearing loss.
Let’s briefly consider these components one by one.
Understanding and addressing the patient’s hearing predicament. Addressing a patient’s hearing predicament entails not only performing diagnostics and providing appropriately fitted hearing aids, but also addressing those communication situations in which a patient would like to experience more success. For example, if a patient wants to converse more successfully with a grandchild, then the plan should include a means to enhance those conversations. If a patient wants to recognize speech better in the presence of background noise, then the plan should include auditory training using competing noise.
Involving the frequent communication partners. How often have we heard the adage that “conversation is a two-way street” and yet have failed to take this into account when designing our hearing treatment plan for a patient? Even when a frequent communication partner, such as a spouse, accompanies a patient to an appointment, the spouse sits in the waiting room reading a magazine or, at most, reads a list of “Do’s and Don’ts” about how to talk to a person who has hearing loss. What doesn’t typically happen is that the partner is given a role to play in the aural rehabilitation process and gains a sense of contributing to the solution. And yet, when family members and other communication partners are involved in the process, patients are most likely to purchase and use hearing aids4 and are much more likely to be satisfied with their hearing treatment plan (see Tye-Murray5 for a review).
Enveloping the patient into a community. Hearing loss can be a very isolating experience and can affect one’s self-identity, self-esteem, and emotional well-being.6 One of the most effective antidotes to these negative consequences is realizing that others are in a similar situation, and being able to connect with these people. Professionals who have performed group aural rehabilitation programs have found this to be true. Indeed, the resounding success of The Hearing Loss Association of America (HLAA), a self-help group of persons who have hearing loss, is due in large part to the sense of community and empowerment that it gives to its members.
Joining the patient on the journey. Due to the constraints of time and economics, many if not most audiologists and hearing care professionals are unable to join the patient on the ongoing journey of having to navigate and remedy the challenges related to hearing loss. That is, once the diagnostics are performed and hearing aids are fitted, and hearing aid counseling is completed, the clinician has limited tools and spends very little time assisting the patient in the communication-improvement journey. At most, an audiologist may be able to send out a clinic “newsletter” or the blanket email to patients, but very few can afford the time to comment on individual patient’s progress or situations.
Yet, contact with a hearing care professional is precisely what many patients most desire. At Washington University, we conducted a study where this proved to be true. We provided auditory training to a group of patients who wanted to receive auditory training. Patients came to us twice a week for a course of eight weeks. When asked, “What did you like best about the training?” the second most popular answer was “Contact with a hearing health care professional”; the first most common answer was, “The sense of helping one’s self.”7
A Solution for Customized Care
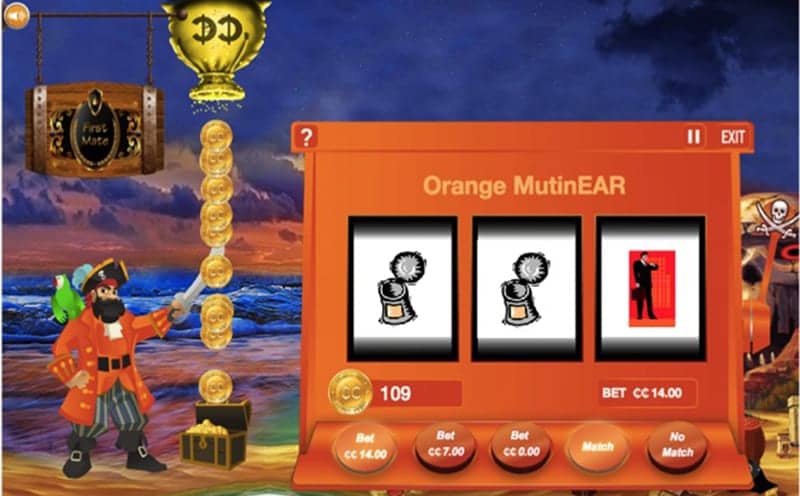
Figure 2. A screen shot from the clEAR game called TreasEAR Island. The patient plays a game that resembles a slot machine and must decide whether a series of three spoken words match the three words illustrated on the game machine. Background noise varies adaptedly with patient performance. The game trains patients to recognize the most frequent words of the language and to make phonetic discriminations. The games are purposely designed to be fun to play so patients might want to play them even if they were not providing benefit.
clEAR, which stands for customized learning: Exercises for Aural Rehabilitation™, is a new web-based auditory training program designed specifically to address these four components. Many hearing care professionals believe that auditory training cannot be fit into the routine protocols of their practice. They believe that it is too expensive and too time-consuming. The clEAR program is designed to address these concerns as it incorporates the four components in Figure 1 in a way that is efficient, effective, engaging, and successful. clEAR provides computerized auditory training in an engaging, game-like format (Figure 2).
clEAR has a proprietary recording and editing system that allows the hearing care professional to use a personal computer microphone to record the voice of a patient’s frequent communication partner speaking the training stimuli. On the same day that the recordings are made (eg, on the day that a patient receives a new hearing aid), the patient can begin receiving auditory training with a frequent communication partner’s voice immediately. The system allows for up to five voices to be recorded, and a voice can be replaced by a new set of recordings made by a different frequent communication partner at any time.
The hearing care professional stays in contact with the patient through an automated email system that is incorporated into the clEAR Professional Provider page, and is able to provide feedback to the patient about performance in training.

Figure 3. A feedback screen that tells patients and their hearing care professional about their performance on the clEAR games. clEAR provides a system for the clinician to quickly send emails of encouragement and feedback to the patient.
Feedback graphs show an array of performance data, such as amount of time trained, percent of correct answers, amount of background noise tolerated, and changes in cognitive indices, such as auditory processing speed (see Figure 3 for an example).
An email message from the hearing care professional might say, “Congratulations Mr. ____, I see you trained ____ minutes today and improved by ___ in the TreasEAR Island game.” In addition to receiving routine customized emails from the clinician, the patient is also enrolled in that clinician’s clEAR community, and receives messages from the audiologist and works toward common goals, which will be generated in the software.
The clEAR solution is only offered through a hearing care professional. If a patient comes directly to the clEAR website, he or she is referred to a local clEAR Professional Provider.
In summary, with the clEAR solution, patients receive the four components of a customized hearing treatment plan:
1) The patient receives customized auditory training;
2) The frequent communication partner is given the important role of recording the training stimuli (and, in the process, learns and practices the principles of “clear speech”);
3) The patient becomes part of a local community of people who have hearing loss, and
4) The patient receives regular contact with the clinician (user benefits are further summarized in Table 2).
-Enhanced speech perception of generic talkers.8,9
-Enhanced speech perception of a frequent communication partner such as a spouse.10
-A partnership with the audiologist and a sense that the audiologist cares about their hearing predicament.7
-Engagement in an auditory training program; 95% of patients who start clEAR training complete it.7
-Reduced perceptual effort when listening.11
Table 2. Benefits a patient is likely to accrue by receiving customized hearing healthcare like that provided with clEAR.
Successful and effective auditory training provided in the context of the model shown in Figure 1 brings enhanced value to a practice. The new clEAR program is designed so auditory training is efficient and profitable, as well. In addition to the above, and beyond providing quality hearing treatment to the patient, clEAR is designed to enhance practice revenue and new patient referrals (to learn more, visit clearworks4ears.com).
Gaming Technology as One Tool in a Successful AR Program
clEAR is just one example of an effective way to provide customized hearing treatment to patients. Many others exist and are extremely useful. Several instruments are available for assessing a patient’s predicament, including the Standard Occupation Classification (SOC),11 the Client Oriented Scale of Improvement (COSI),13 the Hearing Handicap Inventory for Adults (HHIA),14 and the Communication Scale for Older Adults (CSOA)15 (see Sweetow16 for a discussion about how to assess functional communication ability).
Group aural rehabilitation classes, such as those developed by Hickson and her colleagues (the Active Communication Education (ACE) program),17 affords a means to address patient-specific predicaments because participants select the communication difficulties to incorporate into their class work. ACE also affords a means to create a sense of community. The cochlear implant rehabilitation program described by Pedley, Giles, and Hogan18 includes an important role for a patient’s frequent communication partner.
Technology promises a bright future on how audiologists and hearing care professionals might customize hearing treatment. Telepractice already allows for that regular input from the professional, allowing clinicians to reach long-distance from a clinic and provide face-to-face counseling and support.
The world of hearing treatment is no doubt changing. However, with the possibility of customization, the future is bright.
Acknowledgements
This work was supported by the NIH RO1DC008964 grant. Dr Tye-Murray is the CEO of clEAR (customized learning: Exercises for Aural Rehabilitation), which can be found at clearworks4ears.com.
References
-
Fabry D. Disruptive innovation and audiology. Audiology Today. 2015;27(1): 18-23.
-
Windmill IM. 20Q: Prediciting the future of audiology. Audiology Online. April 11, 2016. Available at: http://www.audiologyonline.com/articles/20q-prediciting-future-audiology-16867.
-
Kochkin S. MarkeTrak VIII: 25-year trends in the hearing health market. Hearing Review. 2009;16(11), 12-31. Available at: https://hearingreview.com/2009/10/marketrak-viii-25-year-trends-in-the-hearing-health-market
-
Kasewurm GA. Convincing more patients to get help. Audiology Practices. Available at: http://www.audiologypractices.org/convincing-more-patients-to-get-help.
-
Tye-Murray N. Foundations of Aural Rehabilitation: Children, Adults, and Their Family Members. Stamford, CT: Cengage Learning;2015.
-
Lin FR, Thorpe R, Gordon-Salant S, Ferrucci L. Hearing loss prevalence and risk factors among older adults in the United States. J Gerontology Series A: Biolog Sci and Med Sci. 2011;66(5):582-590.
-
Tye-Murray N, Sommers MS, Mauzé E, Schroy C, Barcroft J, & Spehar B. Using patient perceptions of relative benefit and enjoyment to assess auditory training. J Am Acad Audiol. 2012;23(8):623-634.
-
Barcroft J, Spehar B, Tye-Murray N, Sommers MS. Task and talker-specific gains in auditory training. J Sp-Lang-Hear Res. 2016;59(4):862-870.
-
Barcroft J, Sommers MS, Tye-Murray N, Mauzé E, Schroy C, Spehar B. Tailoring auditory training to patient needs with single and multiple talkers: Transfer-appropriate gains on a four-choice discrimination test. Int J Audiol. 2011;50(11):802-808.
-
Tye-Murray N, Spehar B, Sommers MS, Barcroft J. Auditory training with frequent communication partners. J Sp-Lang-Hear Res. 2016;59(4):871-875.
-
Sommers MS, Tye-Murray N, Barcroft J, Spehar B. The effects of meaning-based auditory training on behavioral measures of perceptual effort in individuals with impaired hearing. Seminars in Hearing. 2015;36(4):263-272.
-
US Department of Labor (DoL). Standard Occupation Classification (SOC). Washington, DC: DoL. Available at: http://www.bls.gov/soc/materials.htm
-
Dillon H, James A, Ginis J. The Client Oriented Scale of Improvement (COSI) and its relationship to several other measures of benefit and satisfaction provided by hearing aids. J Am Acad Audiol. 1997;8:27-43.
-
Newman CW, Weinstein BE, Jacobson GP, Hug GA. The Hearing Handicap Inventory for Adults: psychometric adequacy and audiometric correlates. Ear Hear. 1990;11(6)[Dec]:430-433.
-
Kaplan H, Bally S, Brandt F, Busacco D, Pray J. Communication Scale for Older Adults (CSOA). J Am Acad Audiol. 1997;8(3)[June]:203-17.
-
Sweetow RW. Instead of a hearing aid evaluation, let’s assess functional communication ability. Hear Jour. 2007;(60):26-31.
-
Hickson L, Worrall L, Scarinci N. A randomized controlled trial evaluating the active communication education program for older people with hearing impairment. Ear Hear. 2007;28(2)[Apr]:212-230.
-
Pedley K, Giles E, Hogan A. Adult Cochlear Implant Rehabilitation. Hoboken, NJ:John Wiley & Sons Inc;2005.
Nancy Tye-Murray, PhD, is a professor in the Department of Otolaryngology at Washington University School of Medicine in St Louis, and the CEO of clEAR.
Correspondence can be addressed to HR or Dr Tye-Murray at: [email protected]
Original citation for this article: Tye-Murray N. Gaming Technology for Customized Aural Rehabilitation and Hearing Healthcare. Hearing Review. 2016;23(11):20.?






That’s a cool little project. I would love to play this game even though I don’t even have hearing loss.
Expanding the hearing care offerings by an audiologist offers more value to the hearing impaired person and helps the audiologist to distinguish their care from a business that is just selling hearing aids.