Managing unilateral hearing loss on babies has become a growing aspect of my practice. At the risk of dating myself, I will admit I was educated during a time when it was believed that children would develop normal speech and language with one good ear. We told the parents their children would be fine and sent them on their way.
From experience and compelling data from researchers like Bess, Dodd-Murphy & Parker,1 I now know this is not always the case. Bess et al. found that children with a mild or unilateral hearing loss were three times more likely to be kept back a grade in school and see themselves as socially separate from their peers. With these kids at high risk for academic failure and poor self-esteem, the need for early identification and intervention appears to be as paramount as with their bilateral hearing-impaired peers.
In all that I’ve read and experienced, I’ve yet to be able to reliably predict which child presents more of a risk compared to another. Audiologically speaking, I manage hearing-impaired children aggressively, as if they are all at risk. I approach intervention the same way I’d manage my own child if he had a hearing loss.
There are always key components to those who are more successful than others, like family involvement, motivation, and cognition. However, because judgment and intuition can be wrong, I base recommendations on sound research and past experience. The baby with the asymmetric or unilateral hearing loss has posed more of a problem for me because the literature has been scarce and my relative “successes” with this population have been variable.
However, the recent advent of new technology designed for these configurations of hearing loss is beginning to change my overall assessment of how to manage these kids.
Intervention Strategies for Pediatric Unilateral Losses
Intervention assessment is done case-by-case because family dynamics can vary dramatically. In more recent years, I’ve become a strong advocate of FM technology and fit FM on those children who have profound unilateral hearing loss. I typically fit a monaural hearing aid coupled with a FM system for those kids who had enough residual hearing in the affected ear. However, each intervention plan is individualized to meet the needs of the child and family. Accurately validating outcomes can sometimes be difficult to measure, and compliance tends to be the most significant obstacle. The child with one good or better ear can easily ruse the parent, and the parent does not always find it necessary to utilize the technology because their child “hears.”
The other problem to consider with monaural fittings is the degree of the loss and integrity of the signal. Mark Ross, PhD, does a good job of explaining cochlear dead regions2 and confirms what we already know about older patients who complain about distortion in higher frequencies. [For more information on cochlear dead regions and the TEN test for adults, see Ted Venema’s article in the March 2005 HR.] Although Ross points out that high frequencies are necessary because they convey more of the information required to understand speech, he also states the “audible result of high intensity sounds to the dead regions may be perceived as noise and distortion and actually interfere with speech comprehension.” This really complicates matters for the pediatric audiologist.
Welcome to WiFi
CROS and BICROS configurations have not been a fitting scheme I’ve used for quite some time. Not because I didn’t think the theory was good, but in my view the technology was less than desirable. Most of the kids I fit with CROS technology rejected their device due to poor sound quality and/or loud circuit noise. There were some devices with better sound quality, but the child had to be tethered by a cord that was either too long or too short.
As a pediatric audiologist, cords around the child’s head make me a bit nervous. Even though advances in digital technology have been nothing short of monumental, CROS/BICROS microphones didn’t change from the same old technology and ugly BTE case. The fact is that these devices were not only ugly, they were also “very uncool” in the eyes of a child. Try making a 12-year-old wear one to school.
Needless to say, I was not overly enthusiastic about the introduction of the WiFi Mic either. However, with an increasing number of children with unilateral hearing loss coming to my practice, and current research supporting aggressive audiological management, I felt compelled to try the new device.

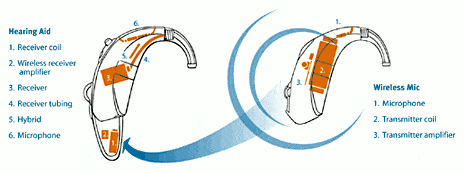
Figure 1. Sounds are processed and transmitted using radio frequency from the wireless microphone on the unaidable ear to the digital hearing aid on the hearing ear.
Although wireless fidelity (WiFi) is not a new concept (probably its most celebrated use is in linking computers to the Internet via wireless connections), the mainstreaming of it for use with hearing instruments in a BICROS fitting is. A BTE-style instrument is worn on the worse ear and transmits the signal using AM frequency to a receiver attached to the battery compartment on the BTE worn on the better side (Figure 1). The system is modular and can be attached to a variety of digital platforms depending on the need for sound processing features. A volume control on the transmitter allows the patient to adjust the signal strength depending on the sound environment.
My first WiFi fitting was a 13-year-old boy with a profound hearing loss in his left ear and a mild-to-severe sloping sensorineural hearing loss in his right ear. He was from a rural Oklahoma town and was home-schooled. His loss had gone undetected until his first visit to our clinic at age 13.
I ordered the WiFi Mic, but it didn’t ship until several months later as it was brand-new technology. In the interim, I fit his right ear with a 6-channel digital hearing aid. It was difficult to get much out of him in terms of how he liked his new amplification; he is a shy 13-year-old and only complained about “static.”
I decided to have him fill out the unaided Abbreviated Profile of Hearing Aid Benefit (APHAB)3 prior to fitting him with the digital hearing instrument. Two months later, he completed the aided APHAB. I then fit him with WiFi, and approximately 2 months later he completed the aided portion of the APHAB again. When I asked him to compare the two fittings, his only response was he liked the WiFi better because “he could hear more.”
After looking at the scored APHABs, it was obvious the WiFi performed much better in all items and subscales: ease of communication, background noise, reverberation, and aversiveness. The biggest discrepancy between the fittings was with ease of communication. He heard more with the BICROS configuration, so he was naturally able to communicate better.

Figure 2. Electroacoustic measurement of output with a Unison Essential BTE in the patient’s better ear as measured by recorded speech.

Figure 3. Electroacoustic measurement of output with a Unitron WiFi Mic in the profound ear as measured by the better ear with live speech in the poorer ear.
I verified the BICROS fitting by first measuring output in the aided side (Figure 2). I then considered the WiFi side by measuring output in the better ear while using live voice and speaking into the poorer ear (Figure 3). Although I realize there is some bleed-over from my voice, for functional purposes I wanted to know how the signal was being shaped into the good ear as it crossed over. The result showed a narrow bandwidth response and a quicker and more precipitous drop in the high frequencies. This measurement, in conjunction with APHAB scores, gave me both objective and subjective proof to qualify this as a successful fit. My first BICROS fitting with WiFi suggested this device was very different from previous technology. Subsequent fittings confirmed it.
I have since fit several kids, as well as adults, with WiFi technology. I don’t hesitate fitting my babies with WiFi due to the compelling data to support early intervention with unilateral hearing losses. It is no longer reasonable to think children with unilateral hearing losses are not at risk for academic failure and poor self-esteem. Knowledge is power, and we have the power to make the changes to change the kids.
We are on the brink of a new era of defining deafness. Hearing-impaired children have the ability to mainstream into a regular classroom with a strong sense of self along with reading and language scores to equal their hearing peers. We must seize the present opportunity placed before us with newborn infant hearing screenings to search, find, and intervene early for all children with hearing loss.
| This article was submitted to HR by Jacqueline Rogers Scholl, MS, a full-time clinical audiologist for the Balance and Hearing Center of Oklahoma. Scholl is also active in legislation relative to educational audiology to benefit children with hearing impairment in her state. She is currently pursuing an AuD, is on the state board for the Alexander Graham Bell Assn, and owns Kid Koncepts, a firm that caters to children with hearing impairment and their parents. Correspondence can be addressed to HR, or Jacqueline Rogers Scholl, MS, 1424 E. 17th Place, Tulsa, OK 74120; email: [email protected]. |
References
1. Bess FH, Dodd-Murphy J, Parker RA. Children with minimal sensorineural hearing loss: Prevalence, educational performance, and functional Status. Ear Hear. 1998;19(5):339-54.
2. Ross, M. Cochlear dead regions. Hearing Loss. 2002;Nov/Dec.
3. Cox R, Alexander G. The abbreviated profile of hearing aid benefit. Ear Hear. 1995;16(2):176-186.