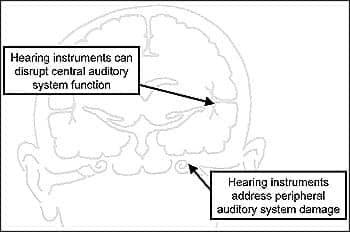
Most hearing care professionals would describe themselves as “patient focused,” meaning they put their patient’s needs and welfare in front of everything else. But, in reality, how involved are patients when it comes to the programming of their hearing instruments, or in having subjective responses to amplification translated into better, more comfortable hearing? Providing that type of direct involvement in each patient’s own hearing instrument programming might truly constitute a “patient-focused” fitting methodology.
Hearing instrument fitting methodologies have recently been categorized according to the underlying theoretical goal, as well as the role of the patient in deriving prescriptive targets. Lindley1 and Lindley et al.2 have described fitting strategies as being either patient-driven (PD) or audiologist-driven (AD). An approach is classified as PD if individual loudness data are obtained from the patient and/or if changes at the initial fitting are made based on the patient’s subjective feedback regarding their perception of amplified sounds. This approach assumes that targets and settings need to be individualized for each patient. On the other hand, an AD approach uses average loudness data in deriving targets, and the patient’s role in determining initial adjustments is limited. It is assumed that the target settings are optimal and that the patient will adjust to sounds that may initially be found unacceptable.
Currently, there is no definitive evidence that one approach, AD or PD, is better than the other for all patients, and arguments can be made for both strategies.1,2 However, a PD approach is appealing because it provides a patient-focused experience. This can potentially have far-reaching effects for increasing patient satisfaction and reducing returns/remakes.
Toward a More PD Approach
Being patient-focused means keeping the patient as an active participant throughout the fitting experience. The process involves them by asking for and incorporating their feedback into the decisions and changes being made. The dispensing professional should be directing the process, but with the patient in the driver’s seat. Evidence in the medical literature that this type of approach results in better health outcomes.3,4
Although the term “patient-driven” describes a philosophy rather than the use of specific procedures or equipment, taking advantage of recent developments in computer hardware and software can enhance the PD approach. Existing PC technology can be leveraged to provide the patient with a multimedia, interactive, individualized experience. This is what the Beltone Audio Verification Environment (AVE.,™ pronounced “avenue”) has been designed to do. The verification system consists of a “surround sound” array of five carefully placed speakers driven by a software program that is now incorporated into Beltone’s SelectaFit fitting software. This makes switching between different programs during a fitting unnecessary. Use of the AVE requires only a sound card and a specific PC-based surround-sound speaker system.
The system can be implemented during every stage of the fitting process. It can be utilized for demonstrating amplification during the difficult “decision” phase, both for new and experienced hearing instrument users. Realistic “real world” sounds can be presented during the delivery session to adjust and fine-tune the hearing instruments, as well as to verify the benefits of amplification and to help set realistic expectations. During follow-up sessions, the system can be used for trouble-shooting and fine-tuning, because sounds and scenarios specific to the patient’s lifestyle can be employed. The patient’s family member or third party also becomes more involved and gains a better understanding of their loved one’s hearing problems when the hearing loss simulator is used.
Audiologically-Derived Auditory Stimuli
 Fig. 1. Screen from the Beltone AVE. Player. The column on the left is the Sound Path, which allows direct access to all the sound selections listed. The graphic on the right is for the “Birds and Stream” selection, which plays bird calls at different intensity levels corresponding to the proximity of the bird selected. The sound of the stream can be turned on or off.
|
Beltone AVE.™ provides a variety of sound selections, as well as supporting graphical representations of many of the selections (Fig. 1). A continuum of auditory stimuli are available, ranging from simple individual sounds or speech in quiet presented through the front speakers to complex sound scenarios incorporating speech mixed with various environmental sounds presented from all five speakers. The auditory stimuli of the system were developed with specific audiologic goals in mind. For example, to meet the goal of demonstrating linear versus WDRC technology, selections with speech or sounds that vary in level between soft and loud were developed. On the other hand, speech at an average conversational level is provided for adjusting amplification to a comfortable listening level. In order to demonstrate directional microphone technology, speech in noise is available with the speech presented from the front while the noise is presented from all around. To verify that overall gain is equally loud in each ear for binaural fittings, noise can be presented from either the front right, left or middle. In order to address reports of difficulties with different types of voices, male, female and children’s voices are provided. The appropriateness of stimuli length was taken into consideration during the system’s development. If the goal of the auditory stimulus is to have the patient identify and repeat back information, then auditory memory can be a factor. Therefore, if the patient is asked to repeat back information from a conversation between two persons, then the selection is limited in length and the information is salient. The system also provides a means of verifying aided loudness via the Sound Matrix, a compilation of various sound selections arranged by category. This is especially useful for verifying that non-linear amplification is providing the appropriate gain for different input levels (i.e., that “soft” sounds are perceived as soft and that “loud” sounds are not uncomfortable). This is important because it may be possible to match a patient’s targets closely with an aid’s performance curves, but still have the patient unhappy with the way particular sounds are perceived. The Sound Matrix includes 36 individual real-world sounds that are categorized by intensity (soft, average, and loud) and by frequency (broadband, high-frequency weighted and low-frequency weighted) as shown in Fig. 2. Sounds that are most likely to be encountered by the patient are chosen and played, individualizing the testing. Ratings of loudness and sound quality are obtained and entered into the software. Changes to the hearing instrument performance curves can be made immediately, and the sounds can be played again to determine if the changes were appropriate. Sounds can also be played while the changes are in progress. In addition to the sounds in the Sound Matrix, a Sound Library contains over 120 individual sounds that can be accessed (Fig. 2). The library can be searched to locate a sound perceived by a patient as being unacceptable. This allows for fine-tuning based on specific complaints during follow-up appointments. Since the AVE. is installed as part of the fitting software, any necessary programming changes are made directly through the software’s “adjustment wizard”, without having to leave the verification software and return to the fitting software. |
|
| Verification Environments & Simulators |
||
 Fig. 3. Verification Environments screen. Selecting an environment brings up an enlarged graphic and stop/play/pause buttons. Simple visual depictions minimize distractions from the listening experience. |
Patients are often overwhelmed when they leave the office after being fit with amplification for the first time. They are confronted with sounds from all around them and may respond by rejecting their new instruments or by becoming discouraged. The Verification Environments were developed in order to address this problem. The seven environments represent a variety of acoustic conditions: a car, a pharmacy, a baseball game, a church, an office, a coffee shop and a kitchen (Fig. 3). Typically, one or two of these are selected that best represent the situations in which the patient will be using their hearing instruments. Presenting the Verification Environments and then discussing the patient’s perceptions of them can help set realistic expectations and confirm that the amplification is appropriate. The recordings were made on location for each of the seven environments using a four-channel sound field microphone and processed in Dolby Pro-Logic™ format to ensure accurate playback from all directions. Filtering using the inverse of the speaker response was also performed to increase the reproduction quality. The goal of the recordings was to provide accurate reproductions of the environments rather than recordings that may be perceived as merely “sounding good,” such as those used in the entertainment industry. A hearing loss simulator is designed to increase the involvement of the patient’s family in the rehabilitative process. The selections currently available for the simulator include conversations with pleasant sounds in the background. A selection is presented to a family member both normally and then processed through the patient’s right- or left-ear audiogram. Graphical representations of the speech spectrum for each condition are displayed for the listener. This demonstration has been shown to be effective, and even dramatic, for some individuals. |
|
Protocols and Set Up |
||
 Fig. 4. Delivery Protocol. This page instructs the practitioner to check for binaural balance using the three available sounds. The ability to adjust the instruments is also provided. |
Step-by-step protocols for demonstration, delivery and follow-up are included to assist the hearing care professional in using the sound selections (Fig. 4). Following the protocols provides direct access to the sound selections, including the Sound Matrix and the Verification Environments at the times when they are most appropriate. The protocols emphasize the interactivity between the patient and the hearing care professional by providing a means to enter the patient’s responses in the software and make changes based on the responses. The Demonstration Protocol is designed to make it easy for the patient to experience amplified sounds even before they decide to purchase hearing instruments. During the Demonstration Protocol, different sounds, types of speech and listening environments can be demonstrated while the patient is wearing actual Behind-the-Ear (BTEs) hearing aids with digital processing and directional microphones configured to their hearing loss. Patients can hear for themselves how the instruments will perform in different environments or for different types of speech. The patient is asked to compare what is heard with and without the aids or with their own aids versus the BTEs. This activity involves them early in the process, which is something desired by many consumers. Step-by-step instructions are provided in the Delivery Protocol to adjust for feedback, overall sound comfort, occlusion and binaural balance. The Sound Matrix is used to verify aided loudness and quality. Programming hearing instruments during delivery becomes a more precise process than trying to determine how much to “tweak” a particular parameter. The last step uses the Verification Environments to confirm the overall fitting and to discuss realistic expectations. The Follow-up protocol allows the dispenser to address specific complaints, such as “the water running in the sink is too loud.” The patient can listen to the “water filling sink” sound selection and then give specific information about its loudness and quality. Improved performance after programming changes can be verified by replaying the selection. Allowing the patient to be intricately involved in the process can result in follow-up visits that are fewer in number, take less time and are more satisfactory for both the patient and the practitioner. Another feature is the incorporation of a set-up procedure. This procedure places the surround-sound speakers in the proper positions so that sound presentation levels are accurate. Included in the software are both a step-by-step procedure for use at initial set-up and a quick procedure for daily checks of levels. Once the levels are adjusted for all the speakers, then the levels of the sound stimuli are deemed appropriate. |
|
Summary
While excellent progress has been made in hearing instrument technology over the last decade, a need continues to exist for the empowerment of the patient during the fitting process. The Beltone AVE. system is designed to provide a comprehensive means of establishing a more patient-driven fitting protocol. It allows the hearing care practitioner to explain what life will be like with new hearing aids, and demonstrate benefit to the patient in the office. Furthermore, the verification system allows for specific patient complaints to be addressed and for the patient to hear their complaints being addressed while in the office. By doing this, the system is designed to increase patient satisfaction by individualizing the fitting while setting realistic patient expectations.
References
1. Lindley G: Adaptation to loudness: Implications for hearing aid fittings. Hear Jour 1999; 52 (11): 50, 52, 56-57.
2. Lindley G, Palmer CV, Durrant J & Pratt S: Adaptation to loudness and environmental stimuli in three newly fitted hearing aid users. J Amer Acad Audiol 2000; 11: 316-322.
3. Eisen SV, Dickey B & Sederer LI: A self-report symptom and problem rating scale to increase inpatients’ involvement in treatment. Psychiatric Services 2000; 51 (3): 349-353.
4. Stewart M, Brown JB, Boon H, Galajda J, Meredith L & Sangster M: Evidence on patient-doctor communication. Cancer Prevention and Control 1999; 3 (1): 25-30.
This article was submitted to HR by Mary E. Meskan, PhD, group leader of research audiology, and Jennifer L. Robinson, MS, research audiologist, with Beltone Electronics Corp., Chicago. Correspondence can be addressed to HR or Mary Meskan, PhD, Beltone Electronics Corp., 4201 W. Victoria St. , Chicago, IL 60646; email: [email protected].