Measured real-ear aided response (REAR) value in 41 adults were significantly different from those predicted by manufacturer fitting software for most of the audiometric frequencies. Few REAR values (<12%) were judged to be clinically similar to software-predicted values, and REAR discrepancies were greater for male ears than female ears. The study suggests that dispensing professionals should conduct their own individual real-ear measures in adult hearing aid fittings until manufacturer software is shown to predict real-ear values with greater accuracy.
Real-ear probe microphone equipment has been commercially available to hearing aid dispensing practices in America for more than 15 years and is used to determine if measured hearing aid performance in the ear matches prescribed performance.1 Some have questioned if real-ear measures are still necessary when fitting digitally programmable analog or digital signal processing (DSP) hearing aids.1-2 Actually measuring real-ear aided responses may be an unnecessary use of clinical time because manufacturers’ proprietary software used to program hearing aids provides an estimation of real-ear hearing aid responses associated with a fitting algorithm.
A study by Hawkins & Cook2 investigated the accuracy of hearing aid performance predicted by hearing aid fitting software, comparing 12 subjects’ measured 2cc coupler and real-ear insertion gain (REIG) values to hearing aid fittings simulated by manufacturers’ fitting software. The authors reported that fitting software over-estimated the actual gain of hearing aids, especially in lower and higher frequencies, and that hearing aids should not be expected to provide the amount of high frequency gain suggested by fitting software.
The following study, which is adapted with permission from a more comprehensive article that appeared in the International Journal of Audiology,3 further examines how accurately one hearing aid manufacturer’s fitting software predicted real-ear aided responses (REAR) for one digital behind-the-ear (BTE) hearing aid. Real-ear aided responses were predicted and tested in four conditions: two hearing loss configurations (flat mild and sloping mild-to-moderately-severe) and two input levels (50 dB SPL and 90 dB SPL). The following questions were asked:
- Does ear or gender effect measured REAR values? These issues were investigated to determine if further analyses could be conducted using data collapsed across ear and gender.
- Are the predicted REAR values generated by the fitting software used here accurate?
- What proportion of adult REAR values are different from predicted, by what amount, and at what frequencies?
Results were used to evaluate the appropriateness of using predicted versus actual REAR measures in adult hearing aid fitting.
Methods
Subjects. Participants were 17 men and 24 women with a mean age of 28.7 years (range 19-55 years). Exclusion criteria included the presence of outer ear anomaly, middle ear system pathology, or cerumen such that probe-microphone measures could not be made. Data was obtained from up to 79 ears depending on the measure.
Hearing instrument and program settings. The hearing instruments used were two nine-channel DSP BTE hearing aids of the same model. These aids were programmed using the most recent version of the manufacturer’s proprietary software in NOAH 3.0 platform software. A Madsen Real-Ear Measures module (version 2.41) was used for hearing aid testing.4
Only one manufacturer’s software was used in this study because only one manufacturer was found to meet two requirements. First, the fitting software provided numeric REAR values in addition to graphical REAR data. Second, the transformations and corrections used by the software when determining predicted REAR values were made available to the authors. Of the eight major hearing aid manufacturers contacted, only the manufacturer represented here met both of these requirements.
Two different hearing loss configurations were entered into the NOAH client module. The first was a flat, mild sensorineural hearing loss and the second was a sloping mild to moderately severe hearing loss (Table 1). The features selected for both hearing aids in the software included the following characteristics: #13 tubing with no venting, omnidirectional microphone, expansion off, and noise reduction off. These characteristics matched those of the bent-tube foam insert used to couple the hearing aids to subjects’ ears and allowed accurate REAR measures to be made.5
| Hearing loss configuration | 500 | 750 | 1000 | 1500 | 2000 | 3000 | 4000 | 6000Hz |
| Flat | 35 | 35 | 35 | 35 | 35 | 35 | 35 | 35 |
| Sloping | 25 | 25 | 35 | 40 | 45 | 50 | 55 | 60 |
TABLE 1. Hearing threshold levels (dB HL) for two hearing loss configurations entered into the manufacturer’s software prior to programming two digital signal processing behind-the-ear hearing aids of the same model.
The first BTE was programmed using the flat hearing loss and the manufacturer’s algorithm; the second BTE was programmed using the sloping hearing loss and the manufacturer’s algorithm. The predicted REAR curves for a 50 dB SPL and a 90 dB SPL broadband input for both audiograms were generated. These REAR values were recorded for later comparison to measured REAR values.
Procedures. Informed consent was obtained prior to data collection. Otoscopy was performed. Middle ear pressure, ear canal volume, and static admittance were obtained using a Madsen Electronics Zodiac tympanometer.
For all real-ear testing, the participant was seated one meter from the real-ear soundfield speaker, in the approximate center of the test booth, at least four feet from each wall. All real-ear measures were obtained using a Madsen Electronics headset. This headset was placed on the participant and the probe tube was inserted into the ear canal to a depth of 28 mm medial to the tragus.6 Stimuli and presentation levels used during real-ear measures were the same as those selected in the manufacturer’s software when the predicted REAR values were provided, and the same as those used originally to generate the average transformations used by the software.
Actual REAR values were obtained using the two BTE hearing aids. Each hearing aid was coupled to a bent tube foam insert. When placed in the ear, the foam tip was allowed to completely expand before testing continued. First a 50 dB SPL and then a 90 dB SPL FFT speech weighted noise of four seconds duration were presented. The resulting REAR values were recorded using both hearing aids in the ears in which real-ear measures could be obtained. The REAR values for all ears tested in the four conditions were recorded.
Results
Descriptive statistics. Otoscopy showed that ear canals were unoccluded in 68 of the 79 ears tested. Minimal cerumen was present in 11 ears; however, the ability to obtain real-ear measures in these ears was not effected. An intact and healthy appearing tympanic membrane was observed in all 79 ears. A Type A configuration was found in 74 of 78 ears; Type AD was found in 2 ears; and Types AS and C were each recorded in one ear only. A tympanogram was not recorded in one subject due to an inability to maintain a hermetic seal.
Mean, SD, and range of ear canal volume (ECV), middle ear pressure (MEP), and static admittance (SA) for male, female, and all subjects were determined. These mean results were within normal limits.7 The mean and standard deviation of the measured REAR values by gender in the four test conditions were determined. The REAR values predicted by the manufacturer’s software were subtracted from each ear’s measured REAR values to produce a difference curve for each ear. The mean difference curves found for male and female subjects in the four test conditions are shown in Figures 1 and 2.
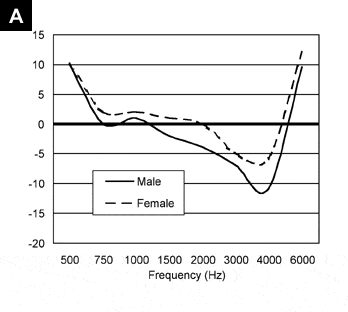
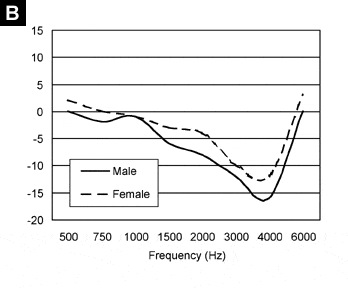
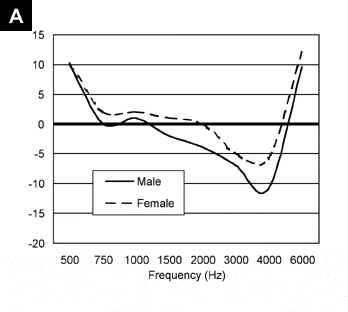
FIGURE 1. Mean difference between measured real-ear aided response (REAR) values and predicted REAR values for male (N=17 subjects, N=31 ears) and female (N=24 subjects, N=47 ears) subjects for a flat mild hearing loss using a 50 dB SPL FFT speech weighted input (A) and a 90 dB SPL FFT speech weighted input (B). Positive values indicate that the measured value exceeded the predicted value while negative values indicate that the predicted value exceeded the measured value. Values of 0 indicate no difference between measured and predicted REAR.
Statistical Analysis. A repeated-measures Analysis of Variance (ANOVA) was conducted to evaluate the effect of ear on measured REAR values to determine if data could be collapsed across ears during subsequent analyses. Results included a non-significant Ear main effect, F(1, 29)=1.439, p=.240, which indicated that measured REAR values were not significantly different for the left and right ears. Therefore, remaining analyses were conducted using data collapsed across ears.
A two-way mixed repeated-measures ANOVA was conducted to evaluate the effect of Gender on measured REAR values to determine if data could be collapsed across genders during subsequent analyses. Multivariate tests were conducted and showed that the Frequency x Gender interaction effect was significant [Wilkes’s Ï=.761, F(7,55)=2.469, p=.02]; the partial eta squared value (.239) denoted a mild relationship between Frequency and Gender while the observed power (.828) was high. The between-subjects effect for Gender was significant [F(1, 61)=11.202, p=.001] with a small effect size (partial eta squared= .155) and a high observed power (.909).
Because Gender was found to be a significant factor, eight one-way ANOVAs were conducted (one for each frequency) to determine the frequencies at which measured REAR values differed for male and female subjects. The results of these ANOVAs indicate that at 1500 Hz, 2000 Hz, 4000 Hz, and 6000 Hz, the measured REAR values are statistically significantly different for most or all of the measurement combinations (two hearing loss configurations/two input levels). Additionally, the males’ measured REAR values were lower than the females’ measured REAR values. Because Gender was a significant factor for most of the mid-high frequencies, subsequent analyses were carried out separately for male and female subjects.
One-sample t-tests were then conducted to compare predicted REAR values to measured REAR values for male and female subjects in the four hearing loss configuration/input level combinations. For most of the frequencies tested, the measured REAR value was statistically significantly different from the predicted REAR value for the two hearing loss configurations, the input levels, and genders.
The data were examined to determine how many ears were and how many were not well predicted by the estimated REAR values provided by the manufacturer’s software. For each measurement condition, predicted and measured REAR values were arbitrarily considered to be dissimilar if actual REAR values were more than 3 dB different from predicted at four or more frequencies. Use of this criterion showed that measured REAR values were different from predicted in all but a few ears (Table 2). Across the four hearing loss configuration/input level combinations, no more than 12% of ears had measured REAR values that were well predicted by the manufacturer’s software.
| Measured REAR values | Flat/50 | Flat/90 | Sloping/90 | Sloping/90 |
| Well predicted by software | ||||
| Males | <2%(2) | <2%(1) | 0%(0) | 0%(0) |
| Females | 5%(4) | <2%(2) | 12%(8) | <2%(1) |
| Poorly predicted by software | ||||
| Males | 38%(30) | 39%(31) | 40%(32) | 40%(32) |
| Females | 54%(43) | 57%(45) | 49%(39) | 58%(46) |
TABLE 2. Percentage (and number of ears) of male (N=32 ears) and female (N=47 ears) subjects with measured REAR values that were and were not well predicted by manufacturer’s software. The four measurement conditions were flat mild hearing loss with a 50 dB SPL input (Flat/50) and a 90 dB SPL input (Flat/90); sloping mild-to-moderately-severe hearing loss with a 50 dB SPL input (Sloping/50) and a 90 dB SPL input (Sloping/90). An ear’s measured REAR values were judged not well predicted if they were more than 3 dB different from predicted at four or more frequencies.
In other words, the ability of the hearing aid fitting software to predict REAR values was poor (as defined here) in 88%-98% of the ears tested, depending on the measurement condition.
Discussion
Overall the results of this study indicate that—for the hearing aid model, hearing loss configurations, and input levels used here—the REAR values predicted by the manufacturer’s fitting software were inaccurate for almost all subjects. The difference between actual and predicted REAR values was greater for males than females. In order to determine if this difference was due to immittance characteristics associated with gender, an ad hoc one-way ANOVA in which gender was the between-groups factor was conducted. Results of this analysis showed a significant difference between male and female subjects for ear canal volume (ECV) only [F(2, 76)=33.114, p=.000] with greater ECV for males than females.
Results also showed that, when arbitrary definitions of good and poor REAR predictability were used, the measured REAR values were well predicted in very few ears (Table 2). A large proportion of the measured 90 dB SPL input individual data points exceeded predicted REAR values. Also, mean measured REAR values exceeded predicted REAR values at low (500 Hz-~1000 Hz) and high frequencies (above 4000 Hz) and fell short of predicted values for the mid frequencies (~1500 Hz-4000 Hz) for the four measurement conditions (Figures 1 and 2). These results are consistent with results reported by Hawkins & Cook2 who found that simulated insertion gain poorly predicted measured insertion gain for 12 adult hearing aid users. However, they found that measured high-frequency insertion gain fell short of, rather than exceeded, predicted values.
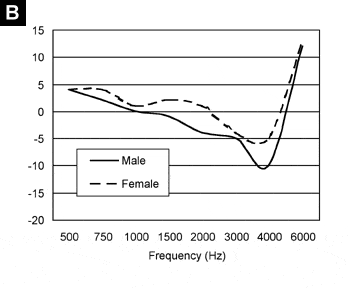
FIGURE 2. Mean difference between measured real-ear aided response (REAR) values and predicted REAR values for male (N=17 subjects, N=32 ears) and female (N=24 subjects, N=47 ears) subjects for a sloping mild-to-moderately-severe hearing loss using a 50 dB SPL FFT speech weighted input (A) and a 90 dB SPL FFT speech weighed input (B). Positive values indicate that the measured value exceeded the predicted value while negative values indicate that the predicted value exceeded the measured. Values of 0 indicate no difference between measured and predicted REAR.
The poor predictability of measured REAR values could have been due to a number of factors. First, the transforms used by manufacturer’s software in order to generate estimates of hearing aid performance in the ear may be inappropriate.1 Second, the use of average Real-Ear to Coupler Difference (RECD) values may effect the hearing aid output predicted in the ear if a hearing aid user’s individual RECD differs from the average RECD used by the software.8-9 Use of average RECD values to predict SPL in the ear will be most useful when the test ear has characteristics similar to those found among subjects used when the average transformations were determined.
Therefore, it is reasonable to measure individual RECD values in the process of hearing aid fitting, at least until the dispensing professional has verified that a given patient’s measured values are consistent with the average RECD used by the fitting software.10-11
Clinical Implications
The discrepancy between predicted and measured REAR values found here suggests that reliance on manufacturer-estimated REAR values—at least for the manufacturer whose technology was used here—is clinically inappropriate, more so for males than females. More studies are needed to determine the predictive accuracy of software used by other hearing aid manufacturers.
If the results found here hold for other manufacturers, and if, as reported, few dispensing professionals routinely use real-ear measures to verify hearing aid fitting, reliance on inaccurate software predictions of real-ear hearing aid performance may partially account for the low satisfaction rates reported by hearing aid users.12-13 That is, results showed that the fitting software typically underestimated hearing aid output in the ear. Insufficient amplification of lower level inputs in hearing aids with automatic volume control could cause hearing aid users to be chronically under-amplified.
Results also showed that over-amplification occurred in many ears when a 90 dB SPL input was used which may contribute to why users continue to claim that hearing aids are too loud.13
Conclusions
Dispensing professionals have the option of fitting hearing aids using REAR values predicted by manufacturers’ fitting software, rather than by using actual measured REARs. This study examined how well one manufacturer’s software was able to predict REARs for a DSP BTE product in 41 adults (N=79 ears) under four conditions (two hearing loss configurations and two inputs). Results showed that, for all ears tested, measured REAR values were significantly different from predicted for most of the audiometric frequencies for all four test conditions. Discrepancies between measured and predicted REAR values were greater in male ears than female ears. Few ears’ REAR values (<12%) were judged to be clinically similar to predicted values.
This study suggests that adult hearing aid fitting protocols should include the use of actual real-ear probe-microphone measures to verify hearing aid fittings. Reliance on predicted real-ear hearing aid performance may result in insufficient output for most hearing aid users, as well as over-amplification of high level inputs for some hearing aid users.
It should be noted that we looked at only one manufacturer’s fitting software; additional studies are needed to determine the predictive accuracy of other software systems. It will also be useful to determine how other manufacturers predict real-ear hearing aid performance and how relevant individual transformations (such as RECD and real-ear-to-dial-difference), measures (real-ear unaided response), and microphone location effects influence the accuracy of predicted real-ear responses.
Acknowledgments
The authors gratefully acknowledge the assistance provided by the developers of the software and technology used in this study, as well as the editor and publisher of the International Journal of Audiology in which a more detailed version of this study appears.3
| Nancy L. Aarts, PhD, is an associate professor of communication at the College of Wooster, Wooster, Ohio, and Carrie S. Caffee, MS, is a clinical audiologist pursuing a doctoral degree at the University of South Alabama, Mobile, Ala. |
Correspondence can be addressed to HR or Nancy L. Aarts, PhD, Department of Communication, 303 E. University, College of Wooster, Wooster, OH 44691; email: [email protected].
References
1. Dillon H, Keidser G. Is probe-mic measurement of HA gain-frequency response best practice? Hear Jour. 2003;56(11):28-30.
2. Hawkins DB, Cook JA. Hearing aid software predictive gain values: How accurate are they? Hear Jour. 2003;56(11):26-34.
3. Aarts NL, Caffee CS. Manufacturer predicted and measured REAR values in adult hearing aid fitting: Accuracy and clinical usefulness. Intl J Audiol. 2005;44:293-301.
4. Madsen Electronics. Aurical audiodiagnostic fitting system reference guide. Copenhagen, Denmark: GN Otometrics; 1998.
5. Mueller G. Probe-mic assessment of digital HAs? Yes, you can! Hear Jour. 2001;54(1):10-17.
6. Searchfield GD, Purdy SC. Probe microphone placement for real ear measurement: Update on a simple acoustic method. Am J Audiol. 1997;6:49-54.
7. Margolis H, Heller J. Screening tympanometry: Criteria for medical referral. Audiol. 1987;26:197-208.
8. Fikret-Pasa S, Revit LJ. Individualized correction factors in the preselection of hearing aids. J Speech Hear Res. 1992;35:384-400.
9. Voss SE, Rosowski JJ, Merchant SN, Thornton AR, Shera, CAP et al. Middle ear pathology can affect the ear-canal sound pressure generated by audiologic earphones. Ear Hear. 2000;21:265-274.
10. Munro KJ, Hatton N. Customized acoustic transform functions and their accuracy at predicting real-ear hearing aid performance. Ear Hear. 2000;21:59-69
11. Zelisko D, Seewald R, Gagne JP. Signal delivery/real ear measurement system for hearing aid selection and fitting. Ear Hear. 1992;13:460-463.
12. Kirkwood DH. Survey finds most dispensers bullish, but not on over-the-counter devices. Hear Jour. 2004;57(3):19-30.
13. Kochkin S. MarkeTrak VI: Consumers rate improvements sought in hearing instruments. The Hearing Review. 2002;9(11):18-22.