Special Issue: Sudden Sensorineural Hearing Loss | December 2003 Hearing Review
Articles in this Special Edition:
- Sudden Hearing Loss: Unique Challenges and Opportunities. An introduction by Maurice H. Miller, PhD, guest editor
- Etiologies and Treatment Options for Sudden Sensorineural Hearing Loss, by Jose N. Fayad, MD, and Antonio De La Cruz, MD
- The Diagnostic and Treatment Dilemma of Sudden Sensorineural Hearing Loss, by Jack J. Wazen, MD, FACS, and Soha N. Ghossaini, MD
- Sudden Hearing Loss: A Team Approach to Assessment, Treatment, and Rehabilitation, by Michael H. Fritsch, MD, Allan O. Diefendorf, PhD, and Michael K. Wynne, PhD
- Steroid Therapy for Sudden Sensorineural Hearing Loss, by Chris Halpin, PhD, and Steven D. Rauch, MD
- Rehabilitative Aspects of ISSNHL, by Maurice H. Miller, PhD, and Jerome D. Schein, PhD
By Michael H. Fritsch, MD, Allan O. Diefendorf, PhD, and Michael K. Wynne, PhD
Hearing loss with a sudden onset may be due to an abnormality involving any part of the auditory system. However, while conductive hearing loss can be sudden, especially with traumatic origins, sudden hearing loss (SHL) refers only to sensorineural losses. Additionally, SHL is almost always unilateral. On the rare occasions when SHL is bilateral (only 2% develop bilateral hearing loss), the hearing loss may affect both ears simultaneously, or be serially spaced months or years apart. Moreover, both ears appear to be equally vulnerable to the occurrence of SHL.
SHL is usually defined as a loss of more than 30 dB over three contiguous frequencies. Some patients can perceive smaller degrees of hearing loss; therefore, 20 dB probably is a better “entry criterion” for working-up a patient.1
The onset of SHL may occur instantaneously or may develop over a period of a few days. Slower hearing loss over more than 3 days usually is described as “rapidly progressive” as opposed to “sudden.”2 In about 50% of individuals, the hearing loss is preceded, accompanied, or followed by vertigo, dizziness, or feelings of unsteadiness. Tinnitus is noted in about 70% of patients. The majority of individuals affected are more than 35 years of age.
The cause for SHL can be found in only 10% to 15% of patients. A number of etiologic factors have been reported. The diverse causes include infectious, vascular, traumatic, immunologic, neurologic, neoplastic, and metabolic problems (Table 1). When no cause is identified, SHL is “idiopathic.”
Most spontaneous recovery of idiopathic SHL starts in the first 2 weeks after onset, with approximately 90% of all improvement occurring within the first 4 weeks after the onset of the hearing loss. In patients who receive medical intervention for known causes, recovery of hearing is related to the time interval between the onset of the hearing loss and the initiation of medical treatment. Therefore, sudden hearing loss, like a sudden loss of vision, is a medical emergency. As such, the longer symptoms persist, the more severe the hearing loss, and the simultaneous occurrence of vertigo all give rise to a poorer prognosis.3 Unfortunately, delay in diagnosis is common because of an insufficient index of suspicion—often due to practitioners attributing the SHL to Eustachian tube dysfunction.
Examination of the Patient
The initial examination of the patient’s complaint should begin with a medical history, followed by an audiologic evaluation and otologic examination. A team approach consisting of an audiologist and otolaryngologist is recommended. A complete history obtained by both professionals may suggest a cause.
It is not uncommon for a patient to report hearing loss after a specific event, such as experiencing physical trauma to the head, straining to lift an object or excessive exertion, barotraumas, or intense (impulse/impact or continuous state) noise exposure. Other patients may report a history of recent or concurrent viral or upper respiratory infections, recent illness or surgeries, or changes in their medications. The exact circumstances and characteristics of the onset of the hearing loss should be determined: Was the loss instantaneous or progressive over several days? The patient may actually describe the exact event and occurrence of hearing loss.

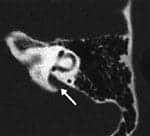
Because SHL often occurs in healthy patients, the general physical examination can be otherwise normal. Otologic examination of the external and middle ears is conducted; however, this examination will be negative in most cases of SHL. Perilymph fistula can be considered only if SHL is closely associated with a well-defined event of physical trauma, exertion, or barotraumas. Lesser trauma to the head, including slight recreational or athletic blows, may raise suspicion for pursuing the diagnosis of enlarged vestibular aqueduct syndrome (VAS) (Figure 1). Acoustic trauma is ruled out based on an absence of reported exposure.

Laboratory studies should be conducted based on the patient’s complaint, history, and suspected etiologies (Table 1). Perhaps the strongest evidence of a viral etiology for SHL comes from studies identifying viruses in the inner ear using immunofluorescence testing (Figure 2). Patients with bilateral SHL may have a systemic disease affecting both ears. Testing for specific systemic problems, such as syphilis or sickle cell disease, is triggered by a thorough history. For patients in whom the history is unrevealing, a broad based hematologic work-up may include a complete blood count (CBC), blood chemistries (eg, creatinine, blood glucose, blood urea nitrogen, uric acid, total bilirubin, alkaline phosphatase, cholesterol, and triglycerides), and serologies (eg, syphilis testing (FTA), Wegner’s granulomatosis (c-ANCA), and other tests). For the patient suspected of autoimmune inner ear disease (AIED), Lymphocyte Transformation testing and erythrocyte sedimentation testing will be revealing. Immune-mediated SHL can be either primary and localized to the inner ear, or secondary to generalized systemic immune disease.

Magnetic resonance imaging (MRI) with gadolinium enhancement is frequently obtained for possible acoustic neuroma (vestibular schwanomma or meningioma), even though these tumors are rare (Figure 3). Because all patients with SHL should receive a retro-cochlear work-up, new approaches to the auditory brainstem response (ie, stacked ABR) offer additional alternatives to clinicians seeking cost-effective diagnostic tools with good sensitivity and specificity for tumor detection.4 Additional neuro-otologic examination including the cranial nerves, cerebellar function, and spontaneous nystagmus may also be carried out.
All patients receive a pure-tone audiogram and other tests to define the hearing loss and rule out pseudohypoacusis. Tympanometry and bone-conduction testing and acoustic reflex measurements are essential for establishing a diagnosis of sensorineural hearing loss. Additionally, the tympanometric technique is ideal for carrying out the fistula test. If a fistula exists, the positive pressure results in nystagmus and creates a sensation of vertigo in the patient. In some settings, the fistula test with an impedance bridge is carried out coupled with an electronystagmography recorder to permit objective determination of nystagmus. Electronystagmography (ENG) itself is useful for persistent dizziness, but is infrequently obtained if dizziness is absent or quickly resolves.
Endolymphathic hydrops is a common histopathologic finding in a limited number of inner-ear diseases, namely Cogan’s syndrome, polyarteritis nodosa, and immune-mediated Meniere’s syndrome. Otoacoustic emissions have increasingly important prognostic value in patients with SHL. It appears that patients with SHL, in the presence of OAEs, experience varying degrees of recovery from their hearing loss.5,6 Electrocochleography may help support the presence of endolymphatic hydrops in the presence of a specific inner ear disease. Finally, because of the wide variation of hearing sensitivity in patients with SHL, the importance of serial audiometric evaluation, including word recognition testing, cannot be overstated.
| INFECTIOUS CAUSES Meningococcal meningitis Cryptococcal meningitis Cytomegalvirus Herpes Rubella Syphilis Toxoplasmosis Human immunodeficiency virus Lassa fever Rubeola Mumps |
VASCULAR CAUSES Vascular disease Vertebrobasilar insufficiency Red blood cell deformity Sickle cell disease Cardiopulmonary bypass Anomalous carotid artery |
TRAUMATIC CAUSES Perilymph fistula Enlarged vestibular aqueduct syndrome (EVAS) Inner ear decompression sickness Temporal bone fracture Surgical complications Inner ear concussion |
| IMMUNOLOGIC CAUSES Primary immune inner ear disease Cogan’s syndrome Wegner’s granulomatosis Lupus erythematosus Polyarteritis nodosa |
NEUROLOGIC/NEOPLASTIC CAUSES Multiple sclerosis Focal pontine ischemia Acoustic neuroma Leukemia Myeloma Metastasis to internal auditory canal Meningeal carcinomatosis |
METABOLIC CAUSES Thyrotoxic hypokalemia Disturbances of iron metabolism Diabetes mellitus Renal failure/dialysisOTHER CAUSES Meniere’s disease Dental surgery Genetic predisposition Pseudohypoacusis |
Table 1. Causes of sudden sensorineural hearing loss.
Medical Treatment Options
The treatment for sudden hearing loss depends on identification of the cause of the hearing loss. For example, when a viral etiology is suspected, systemic antiviral therapy may be warranted. Acyclovir may be recommended for the herpes virus. Antibiotics are recommended for bacterial infections. Surgery may be considered for a perilymph fistula or an acoustic neuroma. In treating a suspected vascular ischemic disorder, the patient may receive Carbogen (a combination of 95% oxygen and 5% carbon dioxide). This treatment is thought to increase the oxygen in the Organ-of-Corti by dilating the cochlear artery. Unfortunately, Carbogen is administered as an inpatient procedure over a period of several days, and this is both inconvenient and expensive. Other therapies, such as plasma volume expander therapy and anticoagulation, remain more controversial.
If the diagnosis of idiopathic SHL is made within the first 7 days of onset, treatment may include a 10-day course of corticosteroid therapy. The action of steroids is diffuse throughout the body and, thus, they often improve systemic inflammatory and immune-mediated conditions. Clinical experience supports giving oral Prednisone for 2-4 weeks to patients with immune-mediated SHL. Medical contraindications to steroid use include existing ulcers, diabetes, and tuberculosis. If hydrops is suspected, patients may benefit from diuretics and a low-sodium (2 gram) diet. The low incidence of SHL, the large number of cases with an undefined cause, and the number of patients with spontaneous recovery makes the study of treatment results difficult at best.
Rehabilitation Options
As medical treatment may or may not be helpful, long-term strategies for rehabilitation should commence early. This approach to patient care underscores the importance of the otologic/audiologic team. Hearing aids, assistive listening devices, and cochlear implants (for cases of bilateral loss) are the optimal treatment options for patients who do not recover their hearing. Hearing aids with multi-memories (and/or volume-controls) offer a larger number of options to fit appropriately the dynamic changes in the hearing loss over time. These systems offer two advantages: 1) Patients have the flexibility to adjust the characteristics of their amplification systems if their hearing changes, and 2) Amplification devices can give patients a sense of control over their communication challenges.
If a bilateral hearing loss progresses to the severe-to-profound range, cochlear implantation becomes an alternative for the patient. After chemotherapy, some patients suddenly lose only the mid-high frequencies and have good residual low-mid frequency hearing. In the partial frequency loss patients, the word recognition is often poor and may be treated by a “partial insertion” cochlear implant at some centers. As in all cases of determining cochlear implant candidacy, a multi-disciplinary team approach will provide the patient with the highest quality care.
Sudden hearing loss is a complex disorder with significant uncertainties and highly variable patient outcomes. A team approach is desirable in order to maximize the diagnostic process, to effectively communicate the risks, benefits, and alternatives of various treatments, and to realize the most beneficial outcomes for long-term patient satisfaction. w
Acknowledgement
Co-author Michael Wynne, PhD, a brilliant and valuable researcher, educator, and clinician in the hearing health care field, died prior to final completion of this article.
| Michael H. Fritsch, MD, Allan O. Diefendorf, PhD, and Michael K. Wynne, PhD, (deceased) are associated with the Dept of Otolaryngology-Head and Neck Surgery at the Indiana University School of Medicine. This issue of HR is dedicated in memory of Dr. Wynne (1954-2003). |
References
1. Hughes GB, Freedman MA, Haberkamp TJ, Guay ME. Sudden sensorineural hearing loss. The Otolaryngologic Clinics of North Amer. 1996;29;3:393-405.
2. Terayama Y, Ishibe Y, Matsushuima J. Rapidly progressive sensorineural hearing loss (rapid deafness). Acta Otolaryngol Suppl. (Stockh). 1988;456:43-58.
3. Mattox DE, Simmons FB. Natural history of sudden sensorineural hearing loss. Ann Otol Rhinol Laryngol. 1977;86:463-480.
4. Don M, Masuda A, Nelson RA, Brackman DE. Successful detection of small acoustic tumors using the stacked derived band ABR method. Am J Otol. 1997;18:608-621.
5. Sakashita T, Minowa Y, Hachikawa K, et al. Evoked otoacoustic emissions from ears with idiopathic sudden deafness. Acta Otolaryngol. 1991;486:66-72.
6. Schweinfurth JM, Cacace AT, Parnes SM. Clinical applications of otoacoustic emissions in sudden hearing loss. Laryngoscope. 1997;107:1457-1463.
Correspondence can be addressed to HR or Michael H. Fritsch, MD, Indiana Univ Medical Center, 702 Barnhill Drive, Suite 0860, Indianapolis, IN 46202; email: [email protected].
Original citation for this article: Fritsch MH, Diefendorf AO, Wynne MK. Sudden hearing loss: A team approach to assessment, treatment, and rehabilitation. Hearing Review. 2003;10(13)[Dec]:24-28.



-300x264.gif)
