Perspective | July 2017 Hearing Review
Comments and real-world comparisons on the recent study about OTC hearing aids
There is much to be learned from the recent IU study on OTC hearing aids. However, as its authors state, the findings are specific to that study and should not be generalized to the population of hearing-impaired individuals at large. A comparison is offered here to an audiology clinic using best practices. Results indicate that removing the professional from the fitting and follow-up process yields significantly lower levels of benefit, satisfaction, and use. If OTC hearing aids become a reality, this should be clearly stated on advertising and packaging; consumers should be informed that research has shown 45% of individuals returned hearing aids that were self-fit. Improving accessibility and affordability is only worthwhile if use and satisfaction are not sacrificed in the process.
There is currently a great deal of discussion and controversy surrounding the topic of over-the-counter (OTC) hearing aids. There is proposed legislation to create a class of hearing aids that would be available to consumers without any professional involvement. Clearly, the goal is to provide greater accessibility at lower cost to the consumer. Less clear is the efficacy of such an approach. Can a consumer self-diagnose hearing loss that is suitable to amplification? Can they self-select and fit an appropriate device? Will the outcomes with an OTC model be similar to the current professional model? The recently published Indiana University (IU) hearing aid outcomes study by Humes et al1,2 addresses many of these questions. This is a “must read” article for anyone involved in working with hearing aids for adults.
The IU Outcome (ABCD) Study
The authors describe their study as the first single-site, placebo-controlled, randomized clinical trial. With the intention of exploring methods to improve the accessibility and affordability of hearing health care, they compared outcomes for 3 groups of subjects:
- Group AB followed audiology best practices;
- Group CD self-selected (consumer decides) their hearing aid without professional input;
- Group P was a placebo group fit in the same manner as group AB, except their hearing aids were programmed to provide no acoustic benefit (ie, an “acoustically transparent” fitting).
To evaluate the effect of purchase price, half of the subjects paid $3,600 and half paid $600 for their pair of hearing aids. A total of 154 subjects completed at least a 6-week trial.
All groups had complete hearing evaluations at the outset of the study. All subjects in this study used as their hearing devices GN Resound Alera 9 mini BTE, open-fit hearing aids, described as “high-end, digital, mini-behind-the-ear hearing aids.” Group AB hearing aids were fit binaurally and programmed for real-ear output matched to NAL NL2 targets; Group P hearing aids were fit binaurally and programmed for transparent insertion gain. Both of these groups were provided the same hour-long orientation session. Group CD selected among choices of hearing aids programmed for three common audiograms. They chose their own tube lengths and domes, and instructions were provided via a video and printed material. No routine follow-up visits were scheduled for any group.
At the end of the initial 6-week period, outcome measures were completed for all groups, and all subjects were asked to declare their intention to keep or return the trial hearing aids. Subjects were informed of their group assignment and given the option of an additional 4-5 week trial. Those who continued were provided the same services as Group AB. The CD group was provided hearing aid orientation and their hearing aids were programmed to NL2 targets. Group P, which had previously received a hearing aid orientation, had their hearing aids reprogrammed to NL2 targets.
The Profile of Hearing Aid Benefit (PHAB) was the primary outcome measure and the Connected Speech Test (CST) was the secondary outcome measure, among several others. The results of the primary measures were not significantly different for Group AB and Group CD. However, both of these groups performed significantly better than Group P. Group AB and P outperformed Group CD on the measures that reflected pretrial training (HASShas; HASSdisp; PHAST). All groups wore their hearing aids 6-7 hours per day. When asked if they planned to keep their hearing aids, responses were substantially different among groups with 81% of Group AB, 55% of Group CD, and 36% of Group P stating they planned to keep their hearing aids.
All hearing aids were thoroughly checked at the end of the first 6-week trial. Many problems were noted, including 88% with twisted or kinked tubing. These problems resulted in less audibility as reflected by comparison of pre-fitting and post-trial 2cc coupler measures of the Speech Intelligibility Index (SII). After all problems were corrected, the added services were provided and the extended trial period began.
Performance for both Groups CD and P improved significantly and were then equivalent to Group AB. In the end, 134 of 154 (87%) of the subjects kept their hearing aids. Despite the improvement after the additional services and trial, the authors felt that the outcomes for the CD group were efficacious and support the use of an OTC model for at least some adults. Purchase price was not found to be a significant factor in the outcomes. However, of those returning their hearing aids, 85% paid the higher price for the hearing aids.
Limitations of the IU Study
The authors describe several limitations of the IU study. They caution that the findings are specific to their unique sample and should not be generalized. It is possible that the casual reader or someone with an agenda to promote the OTC delivery model may not fully embrace these cautions. The most important limitations—which the authors carefully acknowledged—are specifically:
Subjects. The IU report acknowledged they used a sample consisting of white, highly-educated people with a median annual household income greater than $45,000. Most remarkable is that 78% had a college degree and the median education was a masters degree. According to a 2015 US Bureau of the Census report,3 for adults aged 45-64 years and 65 years or older, 32% and 26.7% had at least a bachelors degree and 12.1% and 11.3% had an advanced degree, respectively. It seems likely that the high level of education of the subjects may have influenced outcomes, especially for Group CD. More educated individuals would be expected to be better at independent learning from available instructional materials and applying this to solving their own fitting problems.
Hearing aids. All subjects were fit with GN Resound Alera 9 mini BTE hearing aids, considered a high-end device at the time of this study. The IU authors recognized that this may not be representative of OTC hearing aids. In defense of their choice, they refer to previous research which has failed to show a difference in outcomes with a wide range of technologies.4-6 However, these comparisons were made among FDA-approved products manufactured reliably according to specifications.
There is not currently a class of OTC hearing aids; there is a class of personal sound amplification products, or PSAPs, which arguably are hearing aids by another name. There have been two recent articles that evaluated the wide range of PSAP products available in terms of electroacoustic characteristics, cost, and quality.7,8 The differences among these products are very large with few, if any, having the capabilities of the Alera 9. These PSAPs are probably more typical of the type of device that will be available OTC. Adequate gain, wide bandwidth, suitable compression, safe output limiting, low distortion, and effective feedback management are critical characteristics of any hearing aid technology. These features are available on most current digital hearing aids, regardless of level of technology. Will these characteristics be present on the future generation of OTC devices?
As noted above, the hearing aids for group AB were programmed to match NL2 targets. The hearing aids for Group CD were programmed to three common audiograms and the subjects chose their preferred devices. As Group CD did not have REAR measures completed in Session 1, it is not known how close the pattern of amplification actually was to NL2 targets. However, the fact that the PHAB and CST results were not significantly different between Group CD and Group AB but both were significantly better than Group P indicates there was at least a similar amount of audibility provided. In support of this assumption the 2cc coupler results at the end of the first 6-week trial can be examined. After necessary maintenance was provided the average coupler derived SII for Group CD was only about 2.5% different than for Group AB. Such differences are very commonly found clinically between actual and target real ear measures. It would have been very interesting to see the difference in REAR measures for Group CD before and after programming to NL2 targets for the extended trial.
The IU study compared median audiograms for Group CD subjects to the audiogram for the hearing aid they selected. They reported that subjects chose the best matched hearing aid only 26% of the time. The authors state that there was a clear tendency to select aids with less-than-optimal high-frequency gain. Without real ear measures, it is impossible to know how much NL2 targets actually differed from ear canal levels. Since performance of this group was not significantly different from group AB on the PHAB and CST, again it must be assumed that there was a reasonable amount of gain used.
Audiology best practices. The IU study describes a very detailed “best practice” protocol for hearing evaluation and fitting. However, they acknowledge that “True best practices would also include follow-up appointments during the 6-week trial to adjust the devices in response to patient complaints.” In defense of their decision not to include follow-up visits, they suggest that any post-fitting changes would likely not improve the outcomes and may actually take it away from NL2 targets. They do not discuss any other purpose for follow-up visits.
Some patients need to have hearing aid response adjustments at follow-up visits. These are not always simple gain adjustments that take the patient away from NL2 targets. Adjustments may be needed to help with issues such as sound quality or loudness discomfort. However, there are more reasons that these routine follow-up visits are necessary. Many patients require additional training and counseling on the use of their devices. There is a great deal of information covered with a new hearing aid fitting, and, in many cases, it is better digested in small bites. Some patients have difficulty handling their devices. Some have comfort issues, and some wish to exchange their devices for a different model. More help with telephone communication is often needed.
The lack of follow-up visits is very likely the major contributing factor to the astounding 88% of subjects that had twisted or kinked hearing aid tubing and the consequent reduced SII scores at the end of the 6-week trial. One can only speculate how early in the trial process these problems emerged and if this may have directly contributed to reduced benefit. This problem would have been corrected soon after it occurred with appropriate follow-up visits.
The relatively large number of patients electing to return their hearing aids may also be related to lack of follow-up visits. At the end of the first 6-week trial, subjects were asked if they were likely to keep their hearing aids. Responses were: Group AB, 81%; Group CD, 55%; Group P, 36%. The Hearing Industries Association (HIA) reported a return for credit (RFC) rate of nearly 20% in 2014,9 about the same as for Group AB. It seems the use of best practices for Group AB should have resulted in a lower-than-observed hearing aid return rate.10 Following Session 3B, when subjects were provided the added attention for training (Group CD) and adjustments to the hearing aid settings (Groups CD and P) and the extended 4-5 week trial, the percentage of participants keeping their hearing aids were: Group AB, 89%; Group CD, 84%; and Group P, 88%.
Comparison to a Real-World Audiology Clinic Using Best Practices
Clinic records at Hearing Services & Systems (HSS), Portage, Mich, were searched for similar patients to compare outcomes to the IU study. Over a period extending about 27 months, 57 cases were identified that met the following criteria: new to our office; no previous hearing aid experience; fit with non-occluding RIC type hearing aids (88% with “low- or mid-level” and 12% with “high-level” technology devices); and had completed both pre- and post-fitting surveys.11,12 There were 54% female and 46% male patients with an average age of 71.36 (SD 10.98) years. All patients had been seen for complete hearing evaluation with results showing a typical symmetrical mild-to-moderate sensorineural hearing loss (PTA at 500, 1000, 2000 Hz = 30.72, SD 12.84; HFPTA at 1000, 2000, 4000 Hz = 41.26, SD 12.95).
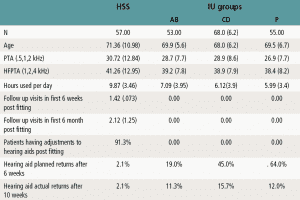
All patients had a hearing aid selection appointment where information was provided of appropriate fitting options along with anticipated benefits and limitations of each. The fitting visit lasted approximately 1 hour and consisted of the physical fitting of the hearing aids, programming to NAL NL2 targets with allowance for patient loudness and sound quality preference, real ear verification with the Audioscan Verifit, and in all but a few cases, one or more follow-up visits. The HSS patient information, along with the three IU groups, is shown in Table 1.
Follow-up visits are bundled into the cost of the hearing aids at HSS so as not to discourage return visits. Of our sample, 95% returned for one or more follow-up visits in the first 6 weeks post-fitting. There were 22% who had two or more visits in the first 6 weeks, and 56% having two or more visits in the first 6 months. During these visits, 91% had some changes made to the hearing aid programming, such as gain, output, adding programs, activating features, etc…Hearing aid data logs read at those times showed the average wear time was about 10 hours per day.
The first item on our hearing aid outcome survey11 (see Appendix A in online version of this article) inquires about wear time, with four response options. There were 88% who responded “most of the day” or “whenever needed,” while only 12% responded “occasionally” or “rarely.” The IU study reports that subjects’ data logs showed they wore their hearing aids 6-7 hours per day. The difference in wear time is likely due to the added care taken in the follow-up visits. It does appear that the AB model may have been “an inappropriately stripped-down version of true best practices that may have minimized differences between it and the CD model.”[p 77]1
RFCs are considered a quality indicator at HSS. During the last 5-year period, HHS had a 2.5% RFC rate considering all types of patients and hearing aids. During the 27-month period noted above, the RFC rate for all patients fit with RIC style hearing aids was 2.1%.
All of HHS patients are sent the Hearing Aid Follow-Up Survey (HAFUS) approximately 2 months post-fitting.11 This survey consists of 18 items addressing issues of use, benefit, and quality of life. For those who do not respond, a prompt, along with a second copy of the HAFUS, is sent one month later. This consistently results in about 80% of surveys returned. In cases where the survey responses are significantly below our normative data, the patient is scheduled for additional follow-up. Benefit is determined by subtracting the results from the 10 communication and quality of life items (items 9-18) on the follow-up survey from the pre-fitting survey results.12 The pre- and post-fitting items are identical except for wording changes to reflect listening with or without hearing aids (Appendix A and B). For scoring, the alpha responses (A-E) are converted to numeric values (1-7), with smaller numbers indicating better outcomes. Scoring of the final item on the pre-fitting survey must be reversed such that a smaller number indicates the patient’s hearing difficulty contributes to a poorer quality of life.
The survey results showed that 87.7% of our patients in this group reported wearing their hearing aids all day or whenever needed. Actual data logs showed wear time of 9.87 (SD 3.46) hours per day. The reported wear time is somewhat lower than the 99% of our normative group, which included 303 experienced and new wearers, who reported wearing their aids most of the day or whenever needed.
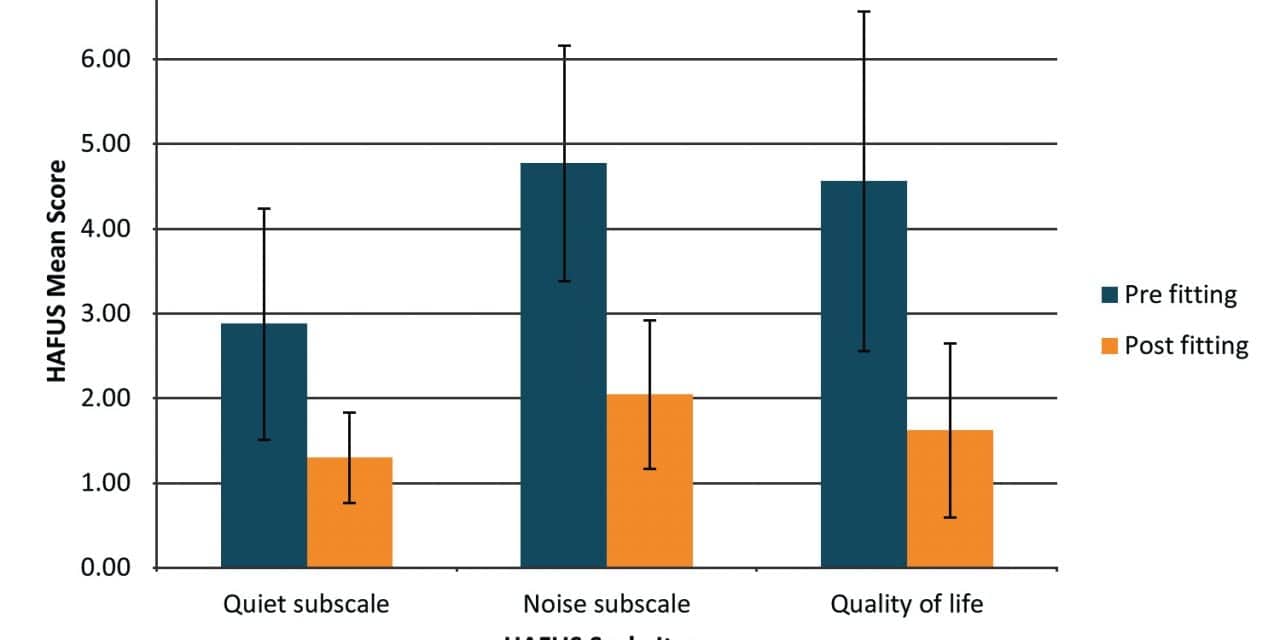
As shown in Figure 1, quality of life was improved by 1 scale unit for 87% of patients and by 2 or more scale units for 80% of patients. Communication was improved in quiet (quiet subscale = average of items 9, 11) by 1.53 (SD 1.60) scale units and in noise (noise subscale = average of items 10, 12, 15, 16) by 2.81 (SD 1.59) scale units. The differences on these three scale items are all significant beyond the .01 level on t-test for paired means with large effect sizes (Cohen’s d ranging from 1.25-1.95). The larger improvement in noise is reflective of the major problems reported by hearing-impaired patients. The smaller improvement in quiet situations occurs because these patients have relatively mild hearing loss causing less difficulty in those situations even without hearing aids. All 10 HAFUS items compared pre- and post-fitting exceed the 95% critical differences, which is less than 1 scale unit.11
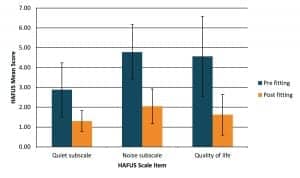
Figure 1. Mean (±1 SD) scores on the HAFUS Quiet subscale (items 9, 11 in survey), the Noise subscale (items 10, 12, 15, 16) and the Quality of life item (item 18). Smaller scores indicate better outcomes.
Discussion
The IU outcome study demonstrated that an OTC model may be efficacious for some individuals. Their Group CD subjects did as well as Group AB subjects on the PHAB and CST. Both the AB and CD groups did better than the P group on all indicators of benefit.
However, on all measures of satisfaction, the CD group was significantly poorer than either the AB or P groups. Strikingly, 88% of all subjects had issues with their hearing aids that required attention to improve audibility by the end of the first 6 weeks. Also, by the end of the initial trial, more than twice as many subjects from the CD group planned to return their hearing aids than the AB group (19% vs 45%). For Group P, 64% initially planned to return their hearing aids. The actual return rate, after audiological involvement and an additional 4-5 week trial, dropped by about 7% for Group AB, 30% for Group CD, and 52% for Group P. These changes are very strong indicators of the benefits of best practices. The findings of this study may have been less favorable for Group CD had the subjects been less educated and the hearing aids less sophisticated. Conversely, the results may have been better for Group AB had they been allowed routine follow-up visits that are typical of best practices.
There is no other study that is directly comparable to the IU double-blind, placebo-controlled, randomized clinical trial. However, there is relevant information available from other investigations that have compared fittings with and without professional involvement. Kochkin10 compared outcomes for people fit with analog mail-order hearing aids with traditional dispenser-fit digital hearing aids. The compelling findings were that the mail order model was efficacious for many people and as good as the traditional “dispenser-fit” model when best practices procedures were limited. However, the results were progressively better for the traditional fitting model as more elements of best practices were followed.
Tedeschi and Kihm8 reported outcomes for a group of 29 subjects with self-reported mild or moderate hearing loss wearing PSAPs and hearing aids. Their subjects selected trial PSAP devices from a diverse group of PSAPs based on printed material, including technical specifications. They then used the selected PSAPs during a 6-week trial. No professional assistance was provided. One-third of participants were dissatisfied with the PSAPs, and 25% stopped using them by the end of the 6-week trial. Eighteen (18) of the subjects continued with Phase 2 of the study when they were fit with hearing aids by a licensed hearing care professional, including counseling and aftercare services. Specific details of the hearing aids were not provided. However, 83% were satisfied with their hearing aids and none had stopped using the devices at the end of the 6-week trial.
The clinical results described above for HSS patients provide strong evidence of the success that may occur for patients fit with hearing aids using best practices, including real ear verification of NAL NL2 targets and follow-up appointments. The patients in this group were of similar age and had similar hearing levels to the IU subjects (Table 1). The HSS patients wore their hearing aids 9.87 hours per day, or 40% longer than the IU group AB. The HSS RFC rate of 2.1% is 17% less than group AB after the first 6-week trial and 9% less after the additional 4-5 week trial. These differences are likely due to the post-fitting care used at HSS but not permitted for IU subjects. In comparing HSS data to the IU group CD, the difference in planned hearing aid returns after the first 6-week trial is 43%. This large difference is indicative of the difference in success that may occur for real-world self-fit hearing aids that have no audiology involvement. The finding that Group CD actual returns were similar to Group AB after the extended trial clearly demonstrates the value of the audiologist in the process.
The hearing aid selection process used by Tedeschi and Kihm8 is probably more like the process that will occur with OTC hearing aids. It is difficult to imagine a “self-serve” retailer that will have a large number of samples available for customers to try on in the store. This would require employee oversight and disinfecting the devices in between customers, both adding to the cost. Probably more likely, a customer will choose from a display and take the devices home to try. Purchasing devices over the Internet will be common. This may be a time-consuming and frustrating process as customers figure out how to use each device and see if it works for them. It seems likely this will result in an even higher level of returned devices than group CD, leaving consumers with the impression that “hearing aids don’t work.”
There is much to be learned from the IU outcome study. It is a landmark paper that provides direction for future research on the efficacy of OTC products. As Humes et al state, the findings are specific to this study and should not be generalized to the population of hearing-impaired individuals at large. Evidence from the IU study and HSS clinical outcomes presented here indicate that removing the hearing care professional from the fitting and follow-up process will result in significantly lower levels of benefit and satisfaction and higher levels of nonuse. This should be clearly stated on advertising and packaging materials if OTC products become a reality. Consumers should be informed that research has shown 45% of individuals returned hearing aids that were self-fit. Improving accessibility and affordability is only worthwhile if use and satisfaction are not sacrificed in the process.
Acknowledgements
Hannah Chase and Wendy Duggan assisted with retrieving data and computer input.

[email protected]
Original citation for this article: Tecca JE. A perspective on the Indiana University OTC outcome study. Hearing Review. 2017;24(7):18-24.
Also see:
For more discussion about this article, see:
Humes L. Letters: Larry Humes Responds to “A Perspective on the Indiana University OTC outcome study.” Hearing Review. 2017;24(8):10.
References
-
Humes LE, Rogers SE, Quigley TM, Main AK, Kinney DL, Herring C. The effects of service-delivery model and purchase price on hearing–aid outcomes in older adults: A randomized double-blind placebo-controlled clinical trial. Am J Audiol. 2017; 26: 53-79.
-
Humes LE, Rogers SE, Quigley TM, Main AK, Kinney DL, Herring C. The effectiveness of two service-delivery models in older adults: A randomized double-blind placebo-controlled clinical trial. Hearing Review. 2017;24(5);12-19.
-
Ryan CL, Bauman K. Educational attainment in the United States: 2015. United States Census Bureau. March 2016. Available at: https://www.census.gov/content/dam/Census/library/publications/2016/demo/p20-578.pdf.
-
Humes LE, Alstrom JB, Bratt GW, Peck BF. Studies of hearing aid outcome measures in older adults: A comparison of technologies and an examination of individual differences. Sem Hear. 2009;30:112-128.
-
Cox RM, Johnson JA, Xu J. Impact of hearing aid technology on outcomes in daily life: The patients’ perspective. Ear Hear. 2016; 37:e224-e237.
-
Johnson JA, Xu J, Cox, RM. Impact of hearing aid technology on outcomes in daily life II: Speech understanding and listening effort. Ear Hear. 2016;37(5):529-540.
-
Smith C, Wilbur LA, Cavitt K. PSAPs vs hearing aids: An electroacoustic analysis of performance and fitting capabilities. Hearing Review. 2016;23(7), 18-22, 24.
-
Tedeschi TJ, Kihm J. Implications of an over-the-counter approach to hearing health care: A consumer study. Hearing Review. 2017;24(3);14-22.
-
Strom KE. Hearing aid Sales increase by 4.8% in 2014; RICs continue market domination. January 20, 2015. Available at: https://hearingreview.com/2015/01/hearing-aid-sales-increase-4-8-2014-rics-continue-market-domination
-
Kochkin S. A comparison of consumer satisfaction, subjective benefit, and quality of life changes associated with traditional and direct-mail hearing aid use. Hearing Review. 2014;21(1):16-26.
-
Tecca JE, Deiters KD. The use of outcome measures in clinical practice: Part 1. Audiology Today. 2017;29(3):50-59.
-
Tecca JE, Deiters KD. The use of outcome measures in clinical practice: Part 2. Audiology Today. 2017; 29(4); In press.
Appendix A. The Hearing Aid Follow Up Survey (HAFUS)
Please take a moment to respond to each item with the answer that best reflects your circumstances. Your answers let us know how your hearing aids help and situations where you are having difficulty. (You will not hurt our feelings if there are problems.)
Hearing Aid Follow-Up Survey
Q1. Please select the item that best describes how you use your hearing aids:
____ I wear my hearing aids most of the day.
____ I wear my hearing aids whenever needed.
____ I wear my hearing aids occasionally.
____ I rarely wear my hearing aids.
Please circle the answers that come closest to your everyday experience. For example, if you strongly agree with a statement, circle “A” for that item.
Q2. My hearing aids are comfortable. A B C D E F G N/A
Q3. My hearing aids are easy for me to handle. A B C D E F G N/A
Q4. My hearing aids are loud enough
for most conversation. A B C D E F G N/A
Q5. My hearing aids keep sound that is already loud
(door slam; dog bark) from becoming uncomfortable. A B C D E F G N/A
Q6. My hearing aids do not squeal/whistle
after they are seated in my ears. A B C D E F G N/A
Q7. My hearing aids have a natural sound
quality for other people’s voices. A B C D E F G N/A
Q8. My hearing aids have a natural sound
quality for my own voice. A B C D E F G N/A
My hearing aids allow me to hear clearly when:
Q9. – talking to 1 other person in a quiet room. A B C D E F G N/A
Q10. – talking to 1 other person in a noisy room. A B C D E F G N/A
Q11. – talking to a small group in a quiet room. A B C D E F G N/A
Q12. – talking to a small group in a noisy room. A B C D E F G N/A
Q13. – talking to 1 other person in a car. A B C D E F G N/A
Q14. – talking on the telephone. A B C D E F G N/A
Q15. – at a meeting or in church. A B C D E F G N/A
Q16. – in a busy restaurant. A B C D E F G N/A
Q17. – watching TV. A B C D E F G N/A
Q18. My hearing aids have improved my
quality of life. A B C D E F G N/A
Please add any comments:
Appendix B. The Hearing Aid Follow Up Survey (HAFUS) communication and quality of life items modified for use as an unaided prefitting measure.
Numbers Q9-Q18 correspond to similar items in the post fitting HAFUS. Item numbers are not used on the actual clinical form.
Please circle the answers that come closest to your everyday experience. If you wear hearing aids, please answer the way you hear without them. For example, if you strongly agree with a statement, circle “A” for that item.
I can hear clearly when:
Q9. – talking to 1 other person in a quiet room. A B C D E F G N/A
Q10. – talking to 1 other person in a noisy room. A B C D E F G N/A
Q11. – talking to a small group in a quiet room. A B C D E F G N/A
Q12. – talking to a small group in a noisy room. A B C D E F G N/A
Q13. – talking to 1 other person in a car. A B C D E F G N/A
Q14. – talking on the telephone. A B C D E F G N/A
Q15. – at a meeting or in church. A B C D E F G N/A
Q16. – in a busy restaurant. A B C D E F G N/A
Q17. – watching TV. A B C D E F G N/A
Q18. My hearing difficulty reduces my
quality of life. A B C D E F G N/A




There’s no need for such a long study that does not speak directly to the attitude of the wearer. Such aids for mild to moderate hearing losses, will be rejected after some use because there will be no perceived benefit. Audiologists will “con” the patient with 3 db excess amplification to create the “wow” effect. These aids will be more accepted for moderate to moderately severe hearing losses. I see a huge return rate for non effectiveness in the performance of such aids, not because of flawed technology, but because of lack of psychology to help the patient in the adaptation process. This is where the audiologist fails regularly.